Medicare #Home health services
- You can use your home health benefits under Part A and/or Part B to pay for home health services. Medicare covers medically necessary part-time or intermittent skilled nursing care, and/or physical therapy, speech-language pathology services, or continued occupational therapy services. A doctor, or certain health care professionals who work with a doctor, must see you face to-face before a doctor can certify that you need home health services. A doctor must order your care, and a Medicare-certified home health agency must provide it.
- Home health services may also include medical social services, part-time or intermittent home health aide services, durable medical equipment, and medical supplies for use at home. You must be homebound, which means:
- • You have trouble leaving your home without help (like using a cane, wheelchair, walker, or crutches; special transportation; or help from another person) because of an illness or injury.
• Leaving your home isn’t recommended because of your condition.
• You’re normally unable to leave your home because it’s a major effort.
- • You have trouble leaving your home without help (like using a cane, wheelchair, walker, or crutches; special transportation; or help from another person) because of an illness or injury.
- You pay nothing for covered home health services. You pay 20% of the Medicare-approved amount, and the Part B deductible applies, for Medicare covered medical equipment. copied from Medicare & You – see brochure in side panel *
- Learn more
Medicare & #HomeHealth Care # 10969
TRUE FREEDOM - Home Health Care
No health questions asked
- Our webpage on Home Health & Long Term Care
- Medicare.Gov Home Health Provider Finder
- Resources to find Home Health & Nursing Care
- FAQ on Home Health Care Nurse - Medical Necessity - Wound Care
- The Medicare Home Health Benefit: An Unkept Promise
- Study Finds Medicare Advantage Patients Experience Worse Home Care Kff
- "Hospital at Home" Programs Improve Outcomes, Lower Costs But Face Resistance from Providers and Payers
- California Guide for Care Givers
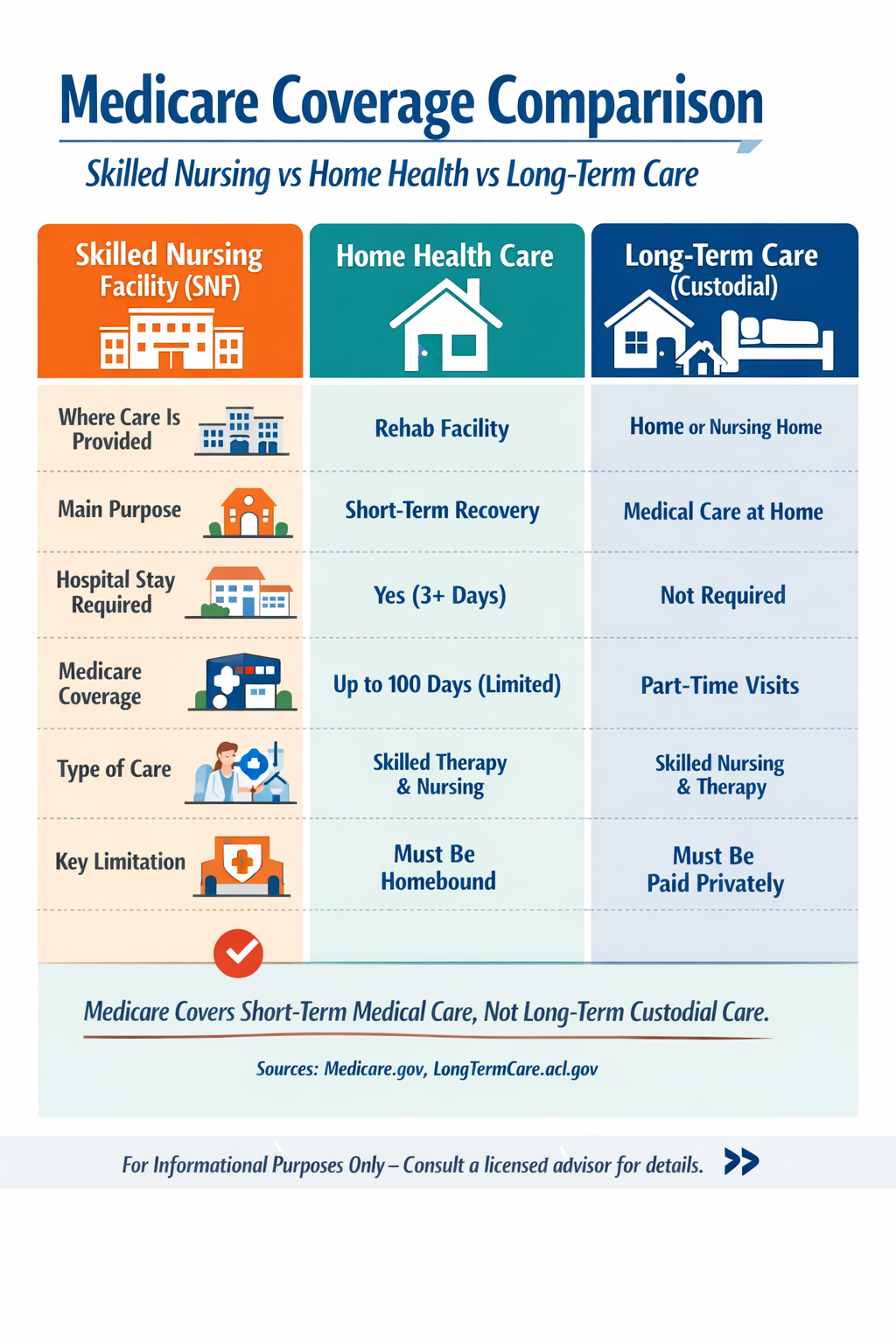
Medicare Coverage Comparison: Skilled Nursing vs Home Health vs Long-Term Care
| Type of Care | Skilled Nursing Facility (SNF) | Home Health Care | Long-Term Care (Custodial) |
|---|---|---|---|
| Where Care is Provided | Nursing facility / rehab center | Your home | Home, assisted living, or nursing home |
| Main Purpose | Short-term recovery after hospital stay | Medical care at home (nurse or therapy) | Help with daily living over time |
| Requires Hospital Stay? | Yes (typically 3+ inpatient days) | No (in many cases) | No |
| Type of Care | Skilled (therapy, IV meds, wound care) | Skilled (nurse visits, therapy) | Custodial (bathing, dressing, eating) |
| Medicare Coverage | Days 1–20: 100% Days 21–100: Copay After 100: Not covered |
Usually covered if medically necessary and homebound | Not covered by Medicare |
| Length of Coverage | Up to 100 days per benefit period | Intermittent / part-time visits | Ongoing / long-term |
| Key Limitation | Stops when skilled care is no longer needed | Must meet “homebound” and medical criteria | Must be paid out-of-pocket or insured |
| Common Misunderstanding | People think it covers long-term stays | People think it includes full-time caregivers | People think Medicare will pay — it won’t |
Bottom line: Medicare is designed for short-term medical care, not long-term living assistance.
Not sure which type of care applies to your situation?
✔ Get help understanding Medicare coverage
✔ Review long-term care planning options
✔ Compare Medicare Supplement plans