Section §125 (Mini Cafeteria) Premium Only Plan (POP)
Employee Contribution – Non Taxable!
POP Premium Only Cafeteria Plan
Introduction
Internal Revenue Code (IRC) Section §125
If your employee’s (and dependent’s) are contributing to your group health plan, their contribution-deduction from their paycheck, for your companies group medical premiums can be tax deductible with a Premium Only Plan – (POP 125) Mini Cafeteria Plan. Internal Revenue Code (IRC) §125 * html .
- Lower taxable AGI – Adjusted Gross Income on the employee’s Tax Return #1040
- PLUS, the POP will lower the employER’s payroll taxes such as
-
-
- FICA *
- FUTA, *
- Medicare Tax, *
- Income Tax Withholding US Code 26 C 21, Publication 535Publication 15-A * 26 U.S. Code § 125 – Cafeteria plans *
- State Disability Insurance (SDI) and
- possibly Worker’s Comp. About.com
-
The way it works, is that your company signs up for a POP plan, with an authorized administrator – vendor, see the links below and on the sides, it’s often the same Insurance Company that your medical coverage is through, but it doesn’t have to be. The cost of the 125 plan is in the neighborhood of $135/year. The administrator-vendor sends you a kit and you distribute the forms and have each employee enroll. The forms do not have to be filed with the government or even the administrator. You just keep them on file in your company records.
The premiums you as the employer is paying for Medical Coverage are already tax deductible for your company is not reportable as income to the employees under Internal Revenue Code §106. The POP plan, allows the portion of the premium that the employee is paying to also be tax deductible, above the line as it lowers Adjusted Gross Income.
See below and the brochures in the margins for more information. Email us for any questions. Send us or enter your census for Group Health Insurance Quotes
To start your companies POP Plan,
Just review the brochures, below, complete the application and return to us, [email protected] . The administrative process and fees (around $150/year) are nominal. It’s a WIN/WIN for both employER, employee and the dependents.
ACA/Obamacare HCR (Health Care Reform) IRC §125 (f) (3) narrows the definition of qualified benefit to exclude Individual Coverage offered through – Covered CA. Notice 2013-54 cuts off employer reimbursement outside of exchange too. Check with us, there might be updates on this.
Brochures
- Health Net
- Flex System POP Info Sheet
- TASC Brochure
- Application 1-888-595-2261 tasc online.com/
- Blue Cross

- Paycheck Manager Calculators – Video Instructions @ 2.16 minutes
- irs.gov Withholding-Calculator (Annual Maintenance?)
- paycheckcity.com/calculator/salary
Just Enter your census or securely send us an excel spreadsheet or a list of employees and get instant proposals for California
More Detail & Brochures
These screenshots were #taken from the POP brochure on TascOnline.com
Read the PDF Brochure – it may be a lot more legible & readable


These screenshots were taken from the POP brochure on Tasconline.com
Read the PDF Brochure – it may be a lot more legible & readable


These screenshots were taken from the POP brochure on Tasconline.com
Read the PDF Brochure – it may be a lot more legible & readable


These screenshots were taken from the POP brochure on Tasconline.com
Read the PDF Brochure – it may be a lot more legible & readable
CORE HSA Health Savings Plan + Section §125 POP Cafeteria Plan
Plan Document Package
- Section 125 POP PDF Document by CoreDocuments.com VIDEO
- What is Section 125?
- Do I need a Section 125 Plan Document for my business?
- How well do free ‘fill-in’ plan document templates work?
- How much do employees save?
- Does a plan bring the employer any tax breaks?
- Who can participate?
- What is a “cafeteria plan”?
- Can I add a health FSA, dependent care FSA, or Health Savings Account?
- Do I have to start a Section 125 plan on January 1?
- What comes with a comprehensive plan document package?
- How do I set up a new Section 125 plan?
- When does a plan document need to be updated?
- How do I order a Core 125 Plan Document package customized for my benefit plan?
- Is there a video on Section 125 plans?
- Where can I find additional resources?
FAQ
- Question Is there any kind of non-discrimination testing in a POP ONLY plan?
. - Answer There are three different non-discrimination tests that must be passed relating to
- 1) eligibility,
- 2) actual contributions and benefits, and
- 3) key employee concentration.
- Employers will get an automatic pass of the three non-discrimination tests if they can satisfy one simple requirement.
- AKA Safe Harbor Rule
- If the ratio of non-highly compensated employees participating in the POP plan compared to the ratio of highly compensated participating in the POP plan is 50% or greater, the employer will be treated as passing all of the non-discrimination tests.
- AKA Safe Harbor Rule
- A key employee is generally an employee who is:
- An officer whose annual pay exceeds $170,000 ($165,000 for 2013); or
- An employee who is either of the following:
- o A 5 percent (or greater) owner of the business; or
- o A 1 percent (or greater) owner whose annual pay is greater than $150,000.
- flexible benefit.com/
- sullivan-benefits.com/Nondiscrimination-Tests-for-Cafeteria-Plans
- Management Carve Outs
- We imagine testing to non be relevant, considering Insurance Company participation rules at generally 75%
. - Question Is this an above or below the line deduction? For Employees ? Employer?
. - Answer Above the line deductions are also known as “adjustments to income” Schedule 1 and are shown above line 11 Adjusted Gross Income of Form 1040.
- In the United States tax law, an above-the-line deduction is a deduction that the Internal Revenue Service allows a taxpayer to subtract from his or her gross income in arriving at “adjusted gross income” for the taxable year. These deductions are set forth in Internal Revenue Code Section 62. A taxpayer’s gross income minus his or her above-the-line deductions is equal to the adjusted gross income. Because these deductions are taken before adjusted gross income is calculated, they are designated “above-the-line.” Thus, those deductions allowed in computing “taxable income” under section 63 of the IRC are “below the line deductions” (thus, adjusted gross income represents “the line”). Above-the-line deductions may be more valuable to high income taxpayers than below-the-line deductions. wikipedia.org
- Income allotted to cafeteria plans is taken directly from an employee’s paycheck before taxes are taken out. These pre-tax contributions can save the employee hundreds—possibly even thousands—of dollars in income taxes and Social Security and Medicare taxes over the course of a year. Turbo Tax * PayCheck *
- A cafeteria plan, including an FSA and POP provides participants an opportunity to receive qualified benefits on a pre-tax basis. It is a written plan that allows your employees to choose between receiving cash or taxable benefits, instead of certain qualified benefits like health insurance for which the law provides an exclusion from wages.
Tax Guides for Employers
EDD California 2024 Employers Guide #DE44 

- Forms & Publications EDD
- FORMS REQUIRED TO GIVE NEW EMPLOYEES
- More workplace protections in 2022 New laws will shield employee health, safety and wages, but some ‘job killer’ bills were axed Los Angeles Times
- Social Security Forms
************************************************************
New Federal Reporting Requirement for Beneficial Ownership Information (BOI)
- Beneficial Ownership Information Reporting Suspended Smart Tax Fin LLC.com
- Effective January 1, 2024, many companies in the United States must report information about their beneficial owners—the individuals who ultimately own or control the company—to the Financial Crimes Enforcement Network (FinCEN), a bureau of the U.S. Department of the Treasury.
- In 2021, Congress enacted the bipartisan Corporate Transparency Act to curb illicit finance. This law requires many companies doing business in the United States to report information about who ultimately owns or controls them.
- Your company may need to report information about its beneficial owners if it is:
- 1. a corporation, a limited liability company (LLC), or was otherwise created in the United States by filing a document with a secretary of state or any similar office under the law of a state or Indian tribe; or
- 2. a foreign company and was registered to do business in any U.S. state or Indian tribe by such a filing.
- FinCEN’s Small Entity Compliance Guide includes checklists for each of the 23 exemptions that may help determine whether your company qualifies for an exemption.
- My CPA's Opinion - this is OVERKILL
Brother - Sister - Sibling Side Pages Subpages
View our website with your Desktop or Tablet for the most information
Links & Reference Material
- ACA Requirement to report value of Health Coverage on W 2
- EDD Taxability of Employee Benefits DE 231 EB
- Our webpage on Management Carve Outs
Broker ONLY
Testimonials
Mr. Shorr,
I’m doing research on using 125 plans for employees who purchase individual insurance, and found your website very helpful, so I thought I would share the following legal analysis of mine, which might be helpful to others:

Mark A. Hall, J.D.
Professor of Law and Public Health
Wake Forest University faculty/profile
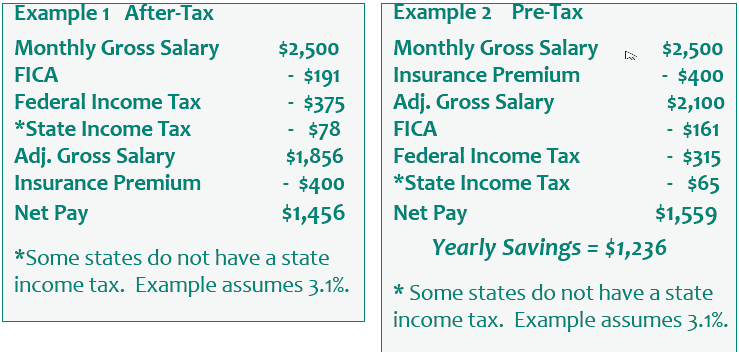









https://www.differencecard.com/blog/how-section-125-plans-work/
What’s ADP’s procedure to deduct the employee’s contribution?
I don’t find the answer in google, guess you’ll have to call For automated support by phone, call 1-844-227-5237
Check these pages on their website
Payroll Deductions
Payroll Fundamentals Workbook-Answers
How to do it in Quick Books
What if an employee is off for a couple of weeks, how do we take the deductions so we can pay the monthly premium to the Insurance Company?
The federal Family and Medical Leave Act (FMLA) requires employers to maintain group health benefits for employees who take FMLA leave. However, employers don’t have to pick up the whole tab unless that is their regular practice. Employers who require employees to pay some portion of their health insurance premiums can continue to require employees to pay that amount while they are off work.
During the time when you aren’t getting paid, however, you’ll have to make other arrangements to pay for your benefits.
One option is to require employees to pay their share of the premium at the same time it would ordinarily be due through payroll deductions. In other words, employers may require employees to pay the premium every payday, as yours has.
The FMLA also allows you and your employer to negotiate a different way to pay premiums. For example, you might prefer to make one large payment rather than having to write a check every two weeks. Or, you might ask whether you can prepay your premiums by having a larger amount withheld from your paycheck in the pay periods leading up to your leave. However, your employer must agree to these alternative methods of payment. NOLO
An employee gets s paycheck every cycle and deductions are made accordingly. If any employee is on vacation the contribution simply goes into minus, it can be balanced out on the next paycheck (response from my wholesaler)
Are all employers who provide health insurance benefits REQUIRED to have a Sect 125 POP plan?
The health insurance benefit premiums could be fully or partially subsidized by the employer.
No. What makes you think that a POP 125 plan is required for all employers?
A POP plan allows the portion paid by the employee to be tax deductible. Here’s a excerpt of the Blue Cross brochure, cited above:
Are you thinking of a full Section 125 cafeteria plan, that offers a full array of benefits, like adoption assistance, child care assistance, life insurance, health savings accounts, flexible spending?