
Management Carve-Outs: Can Employers Give Executives Better Health Insurance?
A management carve-out, sometimes called an executive medical plan or MCO, is when owners, officers, managers, or key employees receive better group health insurance than other employees.
The practical answer for most California small employer health plans is: usually no. Even though ACA Section 2716 enforcement has been delayed pending final regulations, California small group carriers generally do not allow classic executive-only medical carve-outs.
IRS Notice 2011-1 said the nondiscrimination rules for insured group health plans would not be enforced until regulations or other guidance are issued. As of 2026, final regulations still have not been issued. IRS Notice 2011-1
That does not mean carriers will approve a carve-out. In the real world, management carve-outs are usually blocked by carrier rules, participation requirements, contribution requirements, employer eligibility rules, and the requirement that similarly situated employees be treated consistently.
| Email Steve | Set Zoom Meeting | Get Employer Quotes |
What Employers Are Usually Trying To Do
Most employers asking about carve-outs are not trying to do anything improper. They usually want to solve one of these problems:
- Owners want a richer PPO while employees prefer lower-cost HMO coverage.
- Executives want better provider access or out-of-state coverage.
- The employer wants to contribute more for managers than for rank-and-file employees.
- A family-owned business wants coverage mainly for owners or officers.
- Union employees, non-union employees, locations, divisions, or affiliated companies may have different coverage needs.
Some differences may be allowed if they are based on legitimate employment classifications, such as union versus non-union, location, full-time versus part-time, or other bona fide business classifications. Salary, ownership, or favoritism toward highly compensated employees is where the problem usually starts.
Before You Submit an Application
Before you complete a group application, send us the employee census, ownership information, and what you are trying to accomplish. We can help you check whether the proposed arrangement is likely to fit current California carrier rules.
This is especially important if you have common ownership, affiliated companies, multiple locations, union employees, employees waiving coverage, or different contribution levels.
Useful Pages On This Site
- Participation & Contribution Requirements
- Similarly Situated Employees
- ACA Section 2716 Salary Discrimination
- Common Ownership & Affiliated Companies
- California Small Group Carriers
- Employer Group Applications
- Instant Employer Group Proposals
- Section 125 Premium Only Plan
- Section 105 HRA & Reimbursement Plans
- Section 106 Employer Health Insurance Deduction
- 17 Reasons To Buy From Steve Shorr
- Steve Shorr Biography
- Client Testimonials
Other Benefits May Still Work Better For Executives
If the goal is to provide additional benefits for owners or executives, medical insurance is usually the hardest place to do it. Depending on your situation, you may want to look at dental, vision, life insurance, disability income, or long-term care insurance.
Historical & Technical Material
The material below is retained for historical and technical reference. Rules, carrier practices, and enforcement guidance may have changed since some of the older material was written.
Archived versions of this page may be available at the Internet Archive Wayback Machine: View archived versions of this Management Carve-Out page.
Just Enter your census or securely send us an excel spreadsheet or a list of employees and get instant proposals
for all these companies that we are Authorized Agents for in California
§2716 #PROHIBITION OF DISCRIMINATION BASED ON SALARY.
§2716 #PROHIBITION OF DISCRIMINATION BASED ON SALARY.
- §2716 (a) IN GENERAL. The plan sponsor of a group health plan (other than a self-insured plan) may not establish rules relating to the health insurance coverage eligibility (including continued eligibility) of any full-time employee under the terms of the plan that are based on the total hourly or annual salary of the employee or otherwise establish eligibility rules that have the effect of discriminating in favor of higher wage employees.
- (b) LIMITATION. Subsection (a) shall not be construed to prohibit a plan sponsor from establishing contribution requirements for enrollment in the plan or coverage that provide for the payment by employees with lower hourly or annual compensation of a lower dollar or percentage contribution than the payment required of similarly situated employees with a higher hourly or annual compensation. (Patient Protection & Affordable Care Act * SEC. 2716. Section 2716 HR 3590 Page 17)
- Latest Attorney Interpretations of pending final regulations & Guidance
-
Health Care Employment Counsel.co
-
- Please note that the “Final Rule” (2.27.2013 13416 Federal Register Vol 78) allows an
- What and when is a Rule Final??? 33 CFR 1.05-50 –
- What is and how do I know if my plan is Grand Fathered?
Resources & Links
Our Webpage on
- Section §105 -HRA Health Reimbursement & ICHRA
- Cornell Law – code § 105
- highly compensated individual
- (5) Highly compensated individual defined For purposes of this subsection, the term “highly compensated individual” means an individual who is—
- (A) one of the 5 highest paid officers,
- (B) a shareholder who owns (with the application of section 318) more than 10 percent in value of the stock of the employer, or
- (C) among the highest paid 25 percent of all employees (other than employees described in paragraph (3)(B) who are not participants). Cornell Law – code § 105
- (5) Highly compensated individual defined For purposes of this subsection, the term “highly compensated individual” means an individual who is—
- EEOC US Equal Employment Opportunity Commission Employee Benefits
- Can an employer contribute different amounts toward employee medical insurance? Read More People Keep *
- Nondiscrimination in Health and Health Education Programs or Activities, Delegation of Authority Final Rule
What are the nondiscrimination rules under Code §105(h) that will apply to our insured plans if they lose grandfathered status?
- Eligibility Test
- Satisfy at least one of the following nondiscriminatory participation requirements:
- At least 70% of all nonexcludable (see below) employees must actually participate in the plan; or
- If at least 70% of all nonexcludable employees are eligible to participate, then 80% or more of the eligible employees actually participate in the plan; or
- The plan must benefit a classification of employees that the IRS has determined does not discriminate in favor of HCEs Highly Compensated Employee’s using standards that are applied under Code §410(b)
- There are certain employees who can be excluded from consideration when determining if the plan passes the eligibility tests described above, if they are not eligible for coverage and:
- Have not completed at least 3 years of service at the beginning of the plan year.
- Have not attained age 25 at the beginning of the plan year.
- Are part-time or seasonal employees.
- Are covered under a collective bargaining agreement if the benefits are subject to good faith bargaining.
- Are nonresident aliens who receive no income from sources within the US.
- Benefits Test
- Under the subjective nondiscriminatory benefits test, the types and amounts of benefits provided to highly compensated individuals must be provided to all participants. The rule also implies that contributions must be the same for each participating employee. In addition:
- Maximum benefit levels cannot vary based on age, years of service, or compensation. AJG.com *
Links & Resources
- Check our webpage on Participation & Premium Contribution Requirements
- people keep.com offering-different-benefits-for-different-employees
- Highly compensated individual goes to $150k per Notice 2022-55
Management Carve Outs? MCO
- Management Carve Out’s (MCO) Plans, Executive Medical – is where managers, owners and key employees can get better coverage than other workers – similarly situated individuals – employees.
- As of 2023, the status of §2716 Salary Discrimination is up in the air. However, it’s effectively enforced by Insurance Company rules on contribution and participation.
- In the past there must have been bona fide employment-based classifications.
- It’s a very complex issue as Health Care Reform §2716 Salary Discrimination appears to totally prohibit MCO’s. This includes a single employer or affiliated companies (common ownership).
- However, Notice 2011-1 states that §2716 will not be enforced until final rules are issued.
- Health Insurance and most employee benefits the premiums are Tax Deductible with no taxation on the benefits, under IRS Section §106.
- We do not know of any Insurance Companies that will do a Carve Out for other than Union/Non Union employees, where the union employees have coverage through their union Email dated 1.9.2016 11:58 AM Participation rules and all.
- Salary discrimination is still ok for Long Term Care, dental & vision and many other coverages.
Can we give better benefits to #higher wage employees & officers?
- Employers will no longer be able to exclude employees or give better benefits to high wage employees based on salary under §2716, except for Grandfathered Plans (Plans in effect prior to ObamaCare)
- Prior to Health Care Reform, Federal Tax Rules prohibiting Salary Discrimination for Similarly Situated Employees only applied to Self Insured Plans under 26 USC §105 h.
- However, the IRS is not enforcing this rule as final regulations have not been issued. (Notice 2011-1) I googled & googled and as of 1.9.2018, still do not find ANY final regulations! Trumps Executive Order #13765 to minimize the burden of the ACA – Obamacare and #13771 to minimize regulations – one in two out, I guess mean that regulations won’t happen.
- Check out Long Term Care, Dental & Vision and Life Insurance where Executives can STILL have benefits the others don’t!
- Section §106 Health Insurance Deduction is the biggest break there is in the Tax Code, even more than Mortgage Interest.
Health Coverage #Guide
Art Gallagher
Health Care Reform FAQ's
Understanding Health Reform
***********************************
Compliance #Assistance Guide from DOL.Gov Health Benefits under Federal Law
- Health Care Reform Explained Kaiser Foundation Cartoon VIDEO
- Choosing a Health Plan for Your Small Business VIDEO DOL.gov
- ACA Quick Reference Guide California Small Group Employers Revision 2020 Word & Brown
- kff.org/health-policy-101/
- Health Savings Accounts
“Salary Discrimination §2716 – Not enforced”
FAQ
- you state that the IRS is still in a non-enforcement period on this issue until the rules are clarified. Is this still true or is that dated information? If we are currently in a non-enforcement status, can penalties be assess retroactively if we are no longer exempt once the rules are clarified?
- Your question is beyond our pay grade. If you get a plan with us, we will check it out with the Insurance Company, etc. In the meantime, try the Art Gallagher FAQ’s above
- we converted to an individual plan for the remaining employee. The plan stayed with the same insurance co. but not in our companies name. So, would this still be be considered “grandfathered?
- ***I doubt it. See our response in the grandfathering section.
Similarly Situated Individuals
What are Similarly #Situated Individuals?
- Similarly Situated Individuals means that when employees enroll in a employer group health plan if there is any difference in benefits or contribution it must be based on bona-fide employment-based classifications consistent with the employer’s usual business practice, which cannot include any health factors (§1182) or Salary §2716
- similarly situated means adj. with the same problems and circumstances, referring to the people represented by a plaintiff in a “class action,” brought for the benefit of the party filing the suit as well as all those “similarly situated.” To be similarly situated, the defendants, basic facts, and legal issues must be the same, and separate lawsuits would be impractical or burdensome. legal-dictionary
- For example, part-time and full-time employees, employees working in different geographic locations, and employees with different dates of hire or lengths of service can be treated as distinct groups of similarly situated individuals, with different eligibility provisions, different benefit restrictions, or different costs, provided the distinction is consistent with the employer’s usual business practice. The plan also may distinguish between beneficiaries based on, for example, their relationship to the plan participant (such as spouse or dependent child) or based on the age or student status of dependent children. In any case, a plan cannot create or modify a classification directed at individual participants or beneficiaries based on one or more of the health factors or Salary §2716. (dol.gov)
- 29 CFR 2590.702 Health Factors
- Society for HR Management Q & A
- The EEOC Compliance Manual of Employee Benefits, Section 3
- Criteria of “similarly situated employee”
- The work performed
- The responsibility level
- The skills and qualifications required for the respective positions.
- In order to ensure the same criteria are used to determine if the employees are similarly situated, employers must standardize the actual facts regarding employees’:
- Work activities
- Responsibilities
- Skills
- Qualifications.
- In order to effectively evaluate possible differences in similarly situated employees’ compensation, the legitimate factors that influence compensation may include:
- Education
- Experience
- Performance
- Productivity
- Location.World At Work.org/
- Even before health care reform there were generally the same protections for similarly situated individuals under AB 1672 (1992).
- Employer Application for Health Insurance –
Eligibility 
- Who is Similarly Situated? VIDEO
- More on Management Carve Outs…
- Participation and Contribution Requirements
- Insurance Company Employer Health Insurance Applications
- Section 106 Tax Deductibility of Health Insurance Premiums
- Common Ownership – Affiliated Companies – Corporations
- Salary Discrimination §2716 – Not enforced
- Similarly Situated Employees
- Misc.
- To qualify as an accident and health plan, payments under which are excludable from gross income in computing federal income tax liability, a “plan” must benefit all employees or some identifiable class of employees; a plan can be for as few as one employee but there must be some rational basis other than ownership of the corporation to discriminate among employees. American Foundry v. C. I. R., C.A.9 1976, 536 F.2d 289. Internal Revenue 3161
- Similarly Situated Non-COBRA Beneficiaries
- The group of covered employees, their spouses or dependent children who are covered under a group health plan maintained by the employer or employee organization. This group is receiving their benefits under the group plan and not through COBRA continuation coverage. They are most similarly situated to the circumstances of the qualified beneficiary immediately before the qualifying event. (www.dol.gov/)
“Similarly Situated Employees”
- My employer offers drastically different plans based on where employees live. Which business practices must this be consistent with in order to be bona fide? For instance, someone living in Massachusetts has much better coverage than someone living in Connecticut, but I can’t think of a single other business practice that differentiates us.
Thank you!- See the above reference to different geographical locations. We’ve updated this page, so that you can check out other references. Geographical Locations appears to be perfectly legal. Check with your HR department.
- May an ERISA medical benefits plan reimburse retirees under age 65 at a higher amount than retirees aged 65 and older in the same plan and under the same claim situation?
- The issue is tied to the Medicare-eligible retiree vs the retiree dependent under age 65 who is also a participant in another plan.
- I presume you are asking about a plan written under IRS Section 105. Check that page for more detail. Sounds like you should just make sure your plan administrator writes in a clause about other or dual coverage – Medicare Publication 2179. Please be sure to check with competent legal and tax counsel.
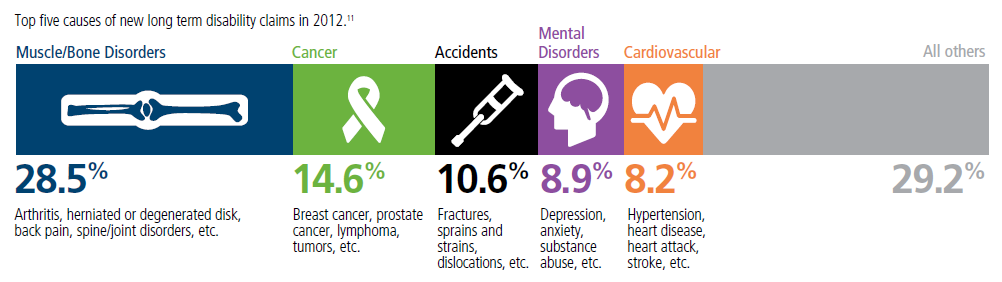
Top 5 - 10 causes of Long Term Disability Claims
Lower back disorders ♦ Depression ♦ Coronary heart disease, arthritis and pulmonary diseases (Met Life) ♦ Disability Can Happen ♦ CDC Statistics
Click here to visit our website on
Consumer Links
- Check out the Option during Annual Open Enrollment 11.15 to 12.15 where there are NO Participation rules!
- Business Expenses Publication #535
- Employer’s Tax Guide to Fringe Benefits Publication #15-B pdf html
- 1.21.2014 New York Times enforcement rules to remain elusive…
- Participation & Premium Contribution Requirements
- Mandate Penalty California – MEC – QHP – 5000 A
Technical Links
Tax Facts on Life & Health Insurance & 2016 Health Reform Facts — Rules on Corp. Officer and Highly Compensated Employees Discrimination, etc. Send us your questions and we can look up the codes and interpretations, but cannot give you tax or legal advise.
Relevant Codes – mentioned on Salary Discrimination – Management Carve Outs – Executive Medical
- IRC §9815 – Additional Market Reforms
- Wraparound coverage to qualify as an excepted benefit Learn More⇒ Federal Register Vol 80 # 52 – 3.18.2015
Historical
Cannot write a carve-out class of a Small Employer Group in the states of Indiana, North Carolina, Ohio, South Carolina, Texas Virginia, Wisconsin or Wyoming (expressly prohibited by their state law). compass consulting inc
Related Pages
Carve Outs & Common Ownership
Management Carve Outs our webpage
- Common Ownership – Affiliated Companies – Corporations
- Our webpage on Section 125 POP Premium Only Plans




