Maternity, Fertility, and IVF Coverage in California
Simple answers to what is covered — and what is not
Short Answer:
In California small group health plans, IVF is not automatically included.
The employer usually must select a specific infertility rider or “INF” plan.
Even when included, coverage depends on plan limits, network rules, and medical necessity.
🤰 Maternity Coverage Is Usually Included
ACA-compliant health plans generally include maternity and newborn care as essential health benefits.
Source: Healthcare.gov essential health benefits
That means pregnancy care, labor and delivery, and newborn care are generally built into compliant individual and family plans.
See our page on maternity and reproductive health
⚠️ Fertility Treatment Is Different from Maternity Care
A plan can cover maternity care and still have limited fertility benefits or no meaningful IVF coverage.
Source: Aetna infertility FAQs
That is why people are often surprised: maternity coverage does not automatically mean IVF coverage.
✔️ What Is Often Covered for Infertility
Depending on the plan, infertility-related benefits may include office visits, diagnostic testing, lab work, medications, and sometimes IUI.
Source: Aetna IUI coverage update
Aetna specifically says IUI is covered on eligible plans, but actual coverage still depends on the employer plan documents.
Source: Aetna infertility FAQs
❗ What About IVF?
IVF is where the biggest misunderstandings happen.
In California, large group plans must cover infertility diagnosis, treatment, and fertility services under SB 729, while small group plans must offer that coverage.
Source: DMHC Winter 2025 newsletter
DMHC’s 2026 guidance also says a large group contract must cover specified fertility services, while the small group offer of coverage must include specified fertility benefits.
Source: DMHC APL 25-021 revised Feb. 23, 2026
So for small employers, the real question is not just “Does California require fertility coverage?” The better question is: “What does this specific small-group plan actually include?”
Scroll down for more information.
🏢 Small Group vs. Large Group in California
- Large group: must cover infertility diagnosis, treatment, and fertility services. Source
- Small group: must offer coverage, but that does not mean every employer selects a rich IVF benefit. Source
- Plan details matter: exclusions, dollar caps, cycle limits, and preauthorization rules can still apply. Source
If you are shopping for employer coverage, start here:
Small Employer Group Health Insurance Plans California
🧠 What About Aetna Small Group in California?
Aetna can be a reasonable choice for infertility-related benefits, but Aetna itself says you need to check the employer’s plan documents for actual infertility coverage.
Source: Aetna infertility FAQs
Aetna also says its clinical policy bulletins are not a guarantee of coverage.
Source: Aetna infertility FAQs
In plain English: some Aetna small-group plans may cover infertility evaluation and IUI, but you should not assume IVF is covered unless the actual plan documents say so.
Source: Aetna IUI page
Related internal page:
Aetna Employer Small Group Health Plans Coverage California
🔍 What to Look for in the Plan Documents
Before you rely on a plan for IVF or fertility services, review the Evidence of Coverage, SBC, rider, or employer benefit summary for:
- Definition of infertility
- Infertility diagnosis coverage
- IUI coverage
- IVF or ART coverage
- Exclusions
- Dollar limits or cycle limits
- Medication coverage
- Preauthorization requirements
- Network or clinic restrictions
Aetna specifically directs members to the employer plan documents and member portal for this information.
Source: Aetna infertility FAQs
Scroll down for more information
Related Pages on Our Website
- Maternity – Reproductive Health – Infertility
- Small Employer Group Health Insurance Plans California
- Aetna Employer Small Group Health Plans Coverage California
- Contact Steve Shorr Insurance
- Schedule a Zoom Meeting
📞 Need Help Reviewing IVF or Fertility Coverage?
We can help you review the plan language before you enroll or before you rely on it for IVF.
Or email us at [email protected]
Note: Benefits vary by carrier, employer contract, renewal date, and plan design. Always verify current benefits in the Evidence of Coverage, Summary of Benefits and Coverage, rider, and official carrier documents.
- Source: Warner Pacific, SB 729 Fertility & Infertility Coverage: Small Group Carrier Coverage Summary, rev. 03/09/26.
- Broker FAQ Sheet
- What you need to know
- Email us [email protected] for a copy
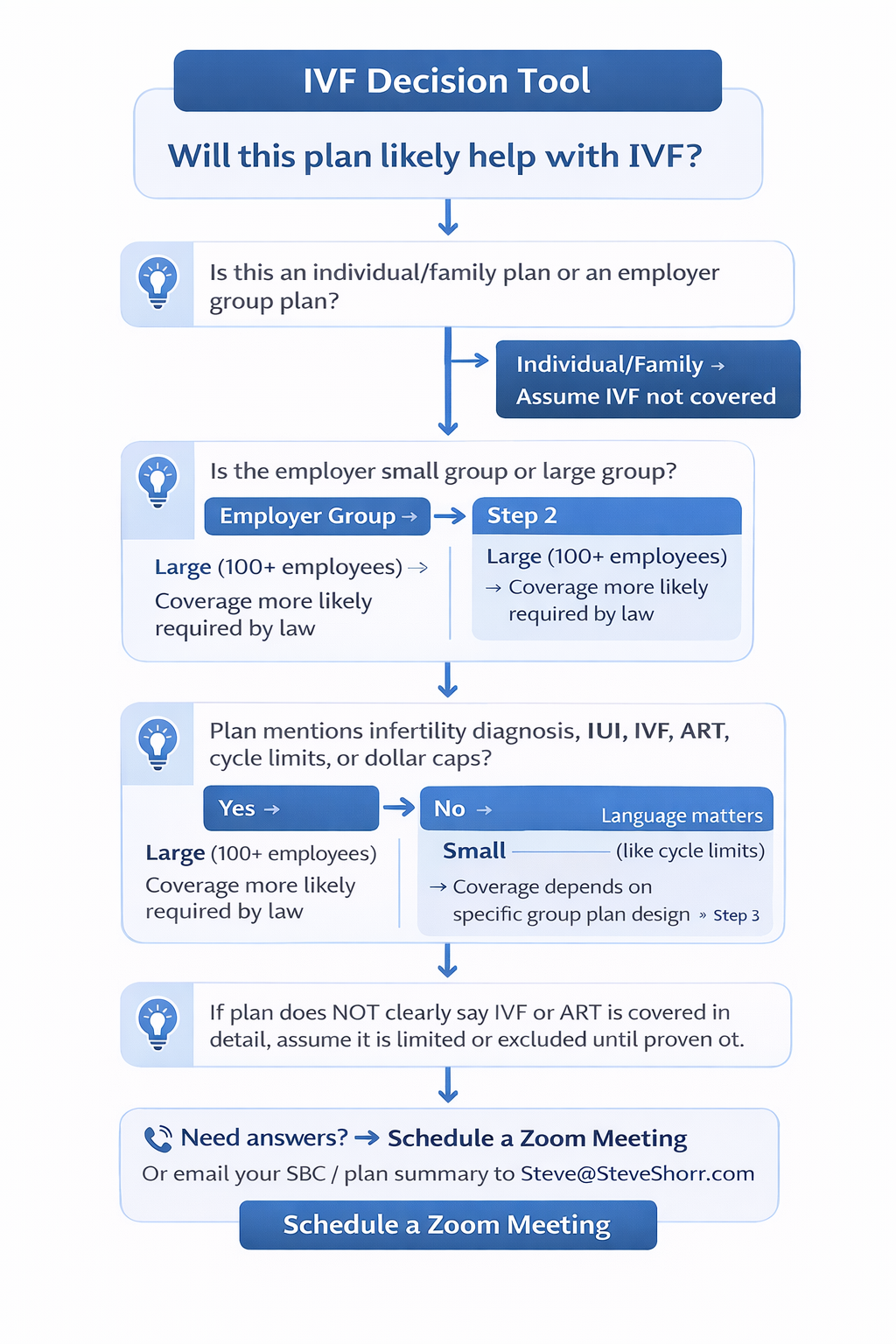
IVF Coverage Decision Tool (California)
Step 1: Individual/Family or Employer Group?
➡️ Individual / Covered CA → IVF usually NOT covered
➡️ Employer Group → Go to Step 2
Step 2: Large (100+) or Small (1–100)?
➡️ Large Group → IVF generally required under SB 729 (2026+)
➡️ Small Group → Go to Step 3
Step 3: Did the employer select an infertility rider or INF plan?
➡️ NO → IVF NOT covered
➡️ YES → Go to Step 4
Step 4: What does the plan actually include?
- IVF specifically listed (not just diagnosis)
- Number of egg retrievals (often 3)
- Embryo transfer rules
- In-network vs PPO access
- Prior authorization required
Final Reality:
Even when IVF is covered, approval depends on medical necessity, plan rules, and carrier review.
Scroll down this page for more information
- Source: Warner Pacific, SB 729 Fertility & Infertility Coverage: Small Group Carrier Coverage Summary, rev. 03/09/26.
- Broker FAQ Sheet
- What you need to know
- Email us [email protected] for a copy
California Small Group IVF Coverage:
What You Can Know Before Enrollment
What to Check Before Enrolling
- Is an infertility rider or INF plan included?
- Is IVF specifically listed (not just diagnosis)?
- How many egg retrievals are covered?
- Are services in-network only?
- Is prior authorization required?
Starting in 2026, California law makes infertility coverage much more important to understand, but the rules are different for large group and small group health plans. For fully insured large group plans, SB 729 requires coverage for the diagnosis and treatment of infertility, including IVF, for plans issued, amended, or renewed on or after January 1, 2026. For fully insured small group plans, infertility and fertility benefits are not automatically included, but carriers must offer at least one small group plan with infertility diagnosis, treatment, and fertility services.
The short answer
You can often tell whether a small group plan has meaningful IVF coverage before enrollment, but only if you review the correct plan version, rider, or infertility option. In many cases, the carrier requires the employer to select a special infertility rider or an “INF” plan at the time of quoting or enrollment. If that option was not selected, IVF may not be covered even if the employer thought it was “available.”
That means the consumer should not have to wait until the policy is active just to know whether the plan includes IVF at all. What usually cannot be guaranteed in advance is whether a specific treatment request will be approved under medical necessity, prior authorization, network, diagnosis, and plan-limit rules.
What agents and consumers should check before enrolling
- Whether the quote or plan name shows an infertility option such as an INF plan or rider.
- Whether the plan covers IVF itself, not just infertility diagnosis or testing. Anthem’s summary, for example, shows a version embedded in Anthem plans that is limited to evaluation only, including diagnostic testing and treatment of underlying medical conditions causing infertility.
- How many retrievals, transfers, or attempts are covered. Several carriers in the summary use limits such as three completed oocyte retrievals, while some have different procedural limits or a one-cycle lifetime maximum.
- Whether the plan is in-network only or offers out-of-network access. Many HMO versions are in-network only, while some PPO versions include both.
- Whether prior authorization is required. Sharp’s summary specifically notes prior authorization by the assigned medical group.
- Whether cost sharing counts toward the plan’s out-of-pocket maximum, since that can vary by carrier and product.
Why “IVF is covered” does not mean the same thing on every plan
One small group carrier may cover IVF, ICSI, GIFT, ZIFT, embryo transfer, and related fertility medications, while another may only cover infertility diagnosis or a much narrower set of procedures. Warner Pacific’s summary shows wide variation among carriers, including different benefit limits, different network rules, and different rider structures.
For example, some summaries show coverage for three oocyte retrievals with unlimited embryo transfers, while another carrier summary shows a one treatment cycle per lifetime limit. That is a huge practical difference for a family trying to plan treatment costs. :
What you can know before the policy is active
Before enrollment, you can usually determine whether the employer selected the infertility rider or INF version, whether IVF is listed as a covered procedure, whether benefits are in-network only, and whether the plan includes important limits such as the number of egg retrievals or embryo transfers. Those are plan design questions, and they should be reviewed from the quote, rider summary, schedule of benefits, or carrier materials before the employer finalizes enrollment. :
What you generally cannot get as an ironclad promise in advance is final approval for a specific person’s treatment. Even when the plan includes IVF, the actual request may still depend on medical necessity rules, documentation, provider network status, diagnosis, and prior authorization. Sharp’s summary, for example, expressly notes prior authorization, and several summaries describe IVF as covered when medically necessary or subject to plan-specific terms.
Practical consumer warning
Do not assume that a small group plan covers IVF just because the carrier offers some infertility option somewhere in its portfolio. In many cases, the infertility option must be affirmatively selected, and if it is selected, it may have to be added to all plans offered by the group. Warner Pacific’s summary repeats that point in multiple carrier sections.
Also, do not assume that “fertility coverage” automatically means unlimited IVF. The carrier summary shows examples of procedural attempt limits, lifetime maximums, plan-specific deductibles, and network restrictions.
Simple way to explain it to clients
Large group: California now generally requires infertility treatment coverage, including IVF, for fully insured large group plans issued, amended, or renewed on or after January 1, 2026.
Small group: The carrier must offer at least one option with infertility coverage, but the employer may need to choose a rider or special INF plan for IVF benefits to be included.
Bottom line: You can often identify whether the plan includes IVF before enrollment, but final approval for treatment still depends on the plan’s rules, the medical facts, and the carrier’s
Need help reviewing a small group IVF option?
Before you enroll, compare the actual rider, INF plan, procedure list, limits, network rules, and prior authorization requirements.
Email your SBC, quote, or benefit summary to [email protected] or schedule a Zoom meeting to review your options.
- Source: Warner Pacific, SB 729 Fertility & Infertility Coverage: Small Group Carrier Coverage Summary, rev. 03/09/26.
- Broker FAQ Sheet
- What you need to know
- Email us [email protected] for a copy
Which California Small Group Plans Actually Cover IVF?
Not all small group health plans include IVF. In many cases, the employer must select a special infertility rider or “INF” plan at the time of enrollment.
Here is a simplified breakdown based on current carrier designs:
- Some plans: Cover infertility diagnosis only (testing, labs, underlying conditions)
- Some plans: Cover limited IVF (example: 1 cycle or specific procedures)
- Some plans: Offer broader IVF coverage (often up to 3 egg retrievals, sometimes unlimited transfers)
Coverage can also vary based on:
- Whether the INF rider is selected
- HMO vs PPO network rules
- Medical necessity requirements
- Prior authorization approval
👉 Bottom line: You cannot assume IVF is covered just because the carrier offers it somewhere. The exact plan and rider selection matter.
- Source: Warner Pacific, SB 729 Fertility & Infertility Coverage: Small Group Carrier Coverage Summary, rev. 03/09/26.
- Broker FAQ Sheet
- What you need to know
- Email us [email protected] for a copy
#SB-729 on how the carriers handle coverage for Infertility
- Source: Warner Pacific, SB 729 Fertility & Infertility Coverage: Small Group Carrier Coverage Summary, rev. 03/09/26.
- Broker FAQ Sheet
- What you need to know
- Email us [email protected] for a copy
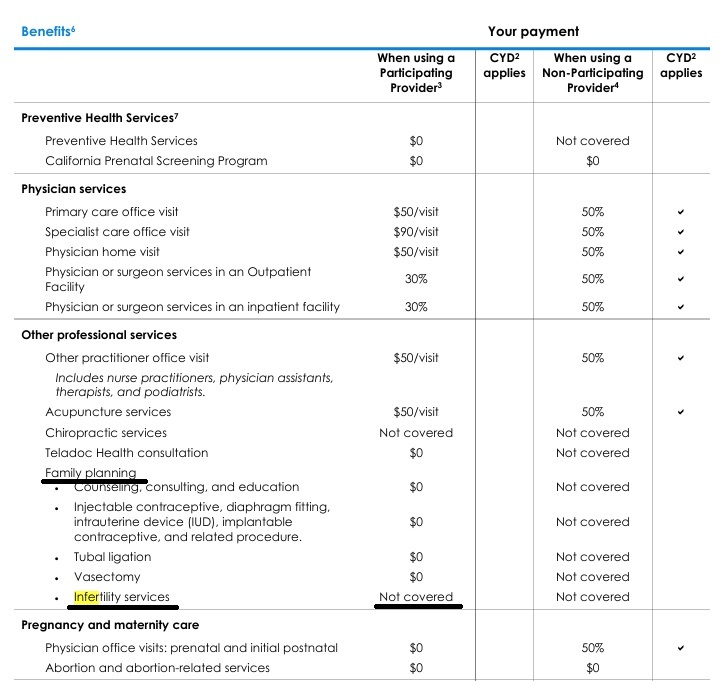
Sample ACA/Obamcare/Covered CA INDIVIDUAL
Silver 70 PPO EOC – Evidence of Coverage – Full Policy
How to read a policy our webpage
Scroll down for Small Employer Group Plans
How is Maternity Covered under
ACA/Health Care Reform/Obamacare
-
- Benefits are available for maternity care services.
- Benefits include:
- Prenatal care;
- Postnatal care; Scroll down for more information.
- Involuntary complications of pregnancy;
- Inpatient Hospital services including labor, delivery, and postpartum care;
- Elective newborn circumcision within 18 months of birth; and
- Pregnancy termination services. G-d Forbid
- See the Diagnostic X-ray, imaging, pathology, and laboratory services and Preventive Health Services sections for information about coverage of genetic testing and diagnostic procedures related to pregnancy and maternity care.
- The Newborns’ and Mothers’ Health Protection Act requires health plans to:
- provide a minimum Hospital stay for the mother and newborn child of 48 hours after a normal, vaginal delivery and
- 96 hours after a C-section.
- The attending Physician, in consultation with the mother, may determine that a shorter length of stay is adequate.
- If your Hospital stay is shorter than the minimum stay, you can receive a follow-up visit with a Health Care Provider whose scope of practice includes postpartum and newborn care. This follow-up visit may occur at home or as an outpatient, as necessary. This visit will include parent education, assistance and training in breast or bottle feeding, and any necessary physical assessments for the mother and child. Prior authorization is not required for this follow-up visit. Page 67 Specimen Policy – Be sure to check YOUR EOC Evidence of Coverage .
- DOL FAQ’s on Newborn and Mothers Health Protection
- Why??? Encouragement to have more babies – Otherwise civilization will end… NPR 4/25/2025 *
- Benefits include:
- References & Links
- Health costs associated with pregnancy, childbirth, and postpartum care
- The high costs of having a baby: New analysis shows childbirth sticker shocks in the U.S
- The staggering financial burden of giving birth — even with insurance
- Women who Give Birth Incur Nearly $19,000 in Additional Health Costs, Including $2,854 More that They Pay Out of Pocket
- My body has changed forever, stretched in ways I’d never imagined since my two pregnancies. My hips have widened, my stomach is softer. There will always be a gap between my abdominal muscles. I have stretch marks, my first and only tattoos. My back aches and feels weaker than before. My boobs are smaller and softer.
- California gives new moms extra Medi-Cal benefits. It can’t say who’s using them
- nbcdfw.com/middle-class-insured-childbirth-crippling-debt
- the mother baby center.org/ labor-induction/
- Blue Shield Mavin
- Blue Shield of California and Maven are here to support fertility and pregnancy journeys every step of the way. With Maven, you and your partner can get access to virtual support for fertility, pregnancy and postpartum. You’ll enjoy 24/7 access to Care Advocates, specialists, mental health support, and content tailored to your experience.
- Confirmation from Blue Shield 12/8/2025 Maven is included within our IFP plans at no additional cost However, please note that infertility treatments (IVF) are not covered under any individual plans.
- Changes under Trump – less testing, screening… Time *
- Health Net Ambetter Maternity & Family Planning
- What is a Midwife – California Health Care Foundation *
- Advantages to Employer if there is less parental stress Kaiser.org *
- Benefits are available for maternity care services.
By submitting the information below , you are agreeing to be contacted by Steve Shorr a Licensed Sales Agent by email, texting or Zoom to discuss Medicare or other Insurance Plans as relevant to your inquiry. This is a solicitation for Insurance
All our Health plans are Guaranteed Issue with No Pre X Clause
Instant Quote & Subsidy #Calculation
There is No charge for our complementary services, we are paid by the Insurance Company.
- Our Quote Engine Takes all the complexity out of using pencil and paper to figure out the premiums per the Obamacare/ACA rules under CFR §1.36B-3 *
- We are authorized Brokers for Dental, Vision & Covered CA get instant quotes direct and in Covered CA with subsidy calculation for:
- Watch our 10 minute VIDEO that explains everything about getting a quote
Infertility Coverage
Employer Group Plans
Infertility on California
Group Employer Plans
- IVF covered in CA new law
- SB 729 Treatment for infertility & fertility services requires large health insurance companies to cover in vitro fertilization
- The bill also expands healthcare benefits to LGBTQ+ families seeking to have children, changing the definition of infertility for insurance purposes to include “a person’s inability to reproduce either as an individual or with their partner without medical intervention.” Read more >>> Los Angeles Times
-
- large and small group health plans issued or renewed after July 1, 2025, must provide coverage for the diagnosis and treatment of infertility and fertility services. It will remove the exclusion of in vitro fertilization from coverage.
- Kaiser Summary
- SB 62 Update CA Benchmark Plan Essential Benefits legislature.ca.gov
- KFF News
- Blue Shield FAQ’s
- Visit our webpage on how to read your EOC Evidence of Coverage – Actual Policy
- time.com//trump-ivf-fertility-insurance
- politico.com//2025/10/25/free-ivf-fizzled-
- white house.gov/2025/10/fact-sheet-ivf-and-high-quality-fertility-care/
- SB 729 Treatment for infertility & fertility services requires large health insurance companies to cover in vitro fertilization
Excerpt from Health Net Plan Guide
- infertility – CA Law? and newborn care.
- §146.130 Standards relating to benefits for mothers and newborns.
- Maternity: Inpatient hospital and ambulatory
- Prescription drug coverage for contraceptives
- Maternity hospital stay
- Sterilization operations and procedures View the Affordable health ca.com page Assembly Bill 1453 (Monning) and Senate Bill 951 (Hernandez). View the California Health and Safety Code, section 1367.005
- ivf specialists.com
- If You’re Poor, Fertility Treatment Can Be Out of Reach
- Federal?
-
IVF – Fertility Treatments
- Even When IVF Is Covered by Insurance, High Bills and Hassles Abound
- Should health insurers cover the cost of fertility treatment?
- Overturning Roe V. Wade: Here’s How It Could Impact Fertility Treatments And IVF
- Aetna Clinical Bulletin Infertility
- Infertility Definition
- May be either of the following:
- A demonstrated condition recognized by a licensed Physician or surgeon as a cause for Infertility; or
- The inability to conceive a pregnancy or to carry a pregnancy to a live birth after a year of regular sexual relations without contraception.
- May be either of the following:
- Fertility preservation services
- Fertility preservation services are covered for Members undergoing treatment or receiving Covered Services that may directly or indirectly cause iatrogenic Infertility. Under these circumstances, standard fertility preservation services
- are a Covered Service.
- Exclusion
- Any services related to assisted reproductive technology (including associated services such as radiology, laboratory, medications, and procedures) including but not limited to
- the harvesting or stimulation of the human ovum,
- in vitro fertilization,
- Gamete Intrafallopian Transfer (GIFT) procedure,
- Zygote Intrafallopian Transfer (ZIFT),
- Intracytoplasmic sperm injection (ICSI),
- preimplantation genetic screening,
- donor services or procurement and storage of donor embryos,
- oocytes, ovarian tissue, or sperm,
- any type of artificial insemination, services or medications to treat low sperm count, or services incident to reversal of surgical sterilization,
- except for Medically Necessary treatment of medical complications of the reversal procedure. Specimen Policy use Ctrl F to find
- Any services related to assisted reproductive technology (including associated services such as radiology, laboratory, medications, and procedures) including but not limited to
- Alabama Republicans want to give IVF doctors immunity after court rules frozen embryos are kids
- Senate Democrats Plan Speedy Action In Defense Of IVF Treatments
- Federal Law
Birth Control
Birth Control – Contraception
-
- Birth control benefits
- Plans in the Health Insurance Marketplace® must cover contraceptive methods and counseling for all women, as prescribed by a health care provider.
- Plans must cover these services without charging a copayment or coinsurance when provided by an in-network provider — even if you haven’t met your deductible.
- Covered contraceptive methods
- FDA-approved contraceptive methods prescribed by a woman’s doctor are covered, including:
- Barrier methods, like diaphragms and sponges
- Hormonal methods, like birth control pills and vaginal rings
- Implanted devices, like intrauterine devices (IUDs)
- Emergency contraception, like Plan B® and ella®
- Sterilization procedures
- Patient education and counseling
- FDA-approved contraceptive methods prescribed by a woman’s doctor are covered, including:
- Plans aren’t required to cover drugs to induce abortions and services for male reproductive capacity, like vasectomies.
TIP To be sure if a specific method is covered by your plan, check your plan’s materials or ask your employer or benefits administrator. - Birth control benefits rules for employer-provided coverage
- If you work for a religious employer
- Health plans sponsored by certain exempt religious employers, like churches and other houses of worship, don’t have to cover contraceptive methods and counseling.
- If you work for an exempt religious employer and use contraceptive services, you may have to pay for them out-of-pocket. Contact your employer or benefits administrator for more information.
- If you work for a non-profit religious organization
- Some non-profit religious organizations — like non-profit religious hospitals and institutions of higher education that certify they have religious objections to contraceptive coverage — don’t have to contract, arrange, pay, or refer for contraceptive coverage.
If your health plan is sponsored or arranged by this type of organization, an insurer or third party administrator will make separate payments for contraceptive services that you use.
- You’ll have access to contraceptive services without a copayment, coinsurance, or deductible when they are provided by an in-network provider.
- Contact your employer or health plan to learn more. health care.gov/ /birth-control-benefits
- Insurers must provide contraceptive coverage at no cost or face potential enforcement action, according to new federal guidance meant to counter reports of coverage denials.
- xyz got caught and has been ordered to reimburse the member — and all others in her situation — for the out-of-pocket costs they incurred. LA Times June 2024
- Why It’s So Hard to the Get Birth Control You Want Covered by Insurance Time Magazine
- HHS, Labor and Treasury put insurers on notice about ACA contraception coverage
- Contraception’s Complains
- Top Biden officials press insurers on contraceptive coverage Advocates for broad coverage say insurers are skirting the rules and denying coverage in some cases
- Birth control benefits
- HHS Warns Insurers Of Penalties If Birth Control Is Not Covered
- California Wants to Snip Costs for Vasectomies
- Our webpage on Preventative Care
- Search Ctrl F * Specimen Policy * for contraception
Instant Term Life Insurance Quote #naaipquote
- Schedule Zoom consultation
- Tools - Calculator to help you figure out how much you should get
- How much life insurance you really need?
Life Insurance Buyers Guide
Abortion
Abortion G-d Forbid
- California governor signs law making abortions cheaper
- Aetna Clinical Policy Bulletins
- Mifepristone (Mifeprex; also known as RU 486)
- CA Department of Insurance Abortion G-d forbid
- kff health news.org/abortion-care-denial-life-threatening-exception-wisconsin/
- kff health news.org/ after-abortion-was-wiped-from-cdc-website-users-now-get-adoption-info