Specialty Medicare Coverage..
DME Durable Medical Equipment, Chiropractic, Hearing Aids, Physical Therapy, Ambulance,
#Durable1 medical equipment (DME)
Medicare Coverage of Durable Medical Equipment Publication 11045
- Medicare covers items like oxygen equipment and supplies, wheelchairs, walkers, and hospital beds ordered by a doctor or other health care provider enrolled in Medicare for use in the home. Some items must be rented. You pay 20% of the Medicare-approved amount, and the Part B deductible applies. If you have a Medi Gap plan, that should pay the 20%! Medicare Advantage, check the summary of benefits or EOC Evidence of Coverage.
- Make sure your doctors and DME suppliers are enrolled in Medicare. Doctors and suppliers have to meet strict standards to enroll and stay enrolled in Medicare. If your doctors or suppliers aren’t enrolled, Medicare won’t pay the claims they submit. It’s also important to ask your suppliers if they participate in Medicare before you get DME. If suppliers are participating suppliers, they must accept assignment (that is, they’re limited to charging you only coinsurance and the Part B deductible for the Medicare-approved amount). If suppliers aren’t participating and don’t accept assignment, there’s no limit on the amount they can charge you.
- To find suppliers who accept assignment, visit Medicare.gov/supplier directory or call 1-800-MEDICARE (1-800-633-4227). TTY users can call 1-877-486-2048. You can also call 1-800-MEDICARE if you’re having problems with your DME supplier, or you need to file a complaint. Copied from Medicare & You – see link in side panel
What about Stair Lifts?
- acorn stair lifts.com
- Medical Necessity of Stair Lifts & Lifting devices Clinical Bulletin?
- Durable Medical Equipment
- Seat Life Mechanisms
- Pride Mobility.com Steps to get Medicare to pay
- hhs.gov research 1989
Guide Dog or Other Service Animal
You can include in medical expenses [but apparently not as durable medical expense] the costs of buying, training, and maintaining a guide dog or other service animal to assist a visually impaired or hearing disabled person, or a person with other physical disabilities. In general, this includes any costs, such as food, grooming, and veterinary care, incurred in maintaining the health and vitality of the service animal so that it may perform its duties. irs.gov/
- Maybe you can get a grant?
Resources & Links
- CMS discontinues medical device forms to ease physician administrative burdens Fierce Health Care * Rev Cycle Intelligence *
- Biden repeals Trump rule that expedited coverage for “breakthrough technology” Modern Health Care * 9.13.2021 prior article * Federal Register 42 CFR Part 405 [CMS-3372-P2] RIN 0938-AT88 *
- Wheelchair users can face hefty costs not covered by insurance, under age 65… LA Times 11.15.2021 *
- Coverage for catheters?
- wikipedia.org/Certificate_of_medical_necessity
#Medicare10050 and You 2025
Spanish
Everything you want to know
- Steve's Video Seminar Introduction to Medicare & You
- 2025 Changes & Updates CA Health Care Advocates 78 page slide show pdf
- Clear View to Medicare Patient Advocate.org - 36 pages
***********
- Your Medicare #Benefits # 10116
- Inpatient ONLY - How Medicare Pays for your Surgery Part A vs Part B Very Well Health.com
- medicare.gov/coverage
- What's Covered App for Smartphones
- Medicare Coverage Database Search
- medicare.gov/procedure-price-lookup
- MLN Items & Services Not Covered Under Medicare
- An Overview-05-19-23 CA Health Care Advocates Hi Cap
- Original Medicare: An Overview CA Health Care Advocates Hi Cap
- 2024 Premiums, Coinsurance & Deductibles – 10-19-23 CA Health Care Advocates Hi Cap
- Supplementing Medicare: An Overview 10-30-20 CA Health Care Advocates Hi Cap
- Enroll in Blue Cross
- Learn about UHC United Health Care
- Enroll in Blue Shield
- SCAN
- Use our scheduler to Set a phone, Skype or Face to Face meeting
- #Intake Form - We can better prepare for the meeting (National Contracting Center)
- TITLE XVIII—HEALTH INSURANCE FOR THE AGED - Medicare AND DISABLE
-
- Welcome to Medicare 2022 Publication # 11095
- Our webpage on Enrolling ONLINE for Medicare Part A Hospital & B Doctor Visits
- Part A Hospital rules for zero premium
- Part B – Doctors – How to sign up – Benefits
- How to apply for Part B when you lose employer coverage - during your special enrollment period # 10012
- Fact Sheet Deciding Whether to Enroll in Medicare Part A and Part B When You Turn 65 CMS.gov 15 pages
- Medicare & You: Deciding to Sign Up for Medicare Part B VIDEO
- CMS form to fill out L 564 E to prove you had Employer Coverage and get a special enrollment period, when you retire. VIDEO
- HI CAP CA Health Care Advocates Medicare Enrollment Periods
FAQ's from Medicare.Gov
#Should I get Parts A & B?
Most people should enroll in Medicare Part A (Hospital Insurance) when they're first eligible, but certain people may choose to delay Medicare Part B (Medical Insurance). In most cases, #How
It depends on the type of health coverage you may have.
- Deciding to Sign Up for Medicare Part B VIDEO
- You must pay your Part B premium every month for as long as you have Part B (even if you don’t use it).
- If I'm low income - are there any breaks?
- Interactive Q & A from IRS on when to sign up for Medicare
- I have coverage through my spouse who is currently working.
- I have retiree coverage (from my former employer or my spouse’s former employer) or COBRA coverage.
- I have TRICARE, and I'm a retired service member.
- I have TRICARE, and I'm an active-duty service member.
- I have CHAMPVA.
- I have End-Stage Renal Disease (ESRD).
- I have Marketplace Covered CA or other private insurance.
- I don't have any of these.
- medicare.gov/should-i-get-parts-a-b
- How to apply for Part B during your special enrollment period # 10012
- Fact Sheet Deciding Whether to Enroll in Medicare Part A and Part B When You Turn 65 15 pages
- FAQ's that we did
Chiropractic Coverage
#Chiropractic coverage in Medicare
- VIDEO explanation Chiropractic
- Here’s how Medicare A & B and the a Typical MAPD Plan. and Medi Gap would pay the 20% that Medicare allows, but leaves as a co payment.
- Medicare Part B pays 80% for spinal manipulation if medically necessary. Thus, Medi Gap and Medicare Advantage only pay, if Medicare does.
- Medicare doesn’t cover other services or tests ordered by a chiropractor, including X-rays, massage therapy, and acupuncture. If you think your chiropractor is billing Medicare for chiropractic services that aren’t covered, you can report suspected Medicare fraud Medicare.gov *
Medical Necessity get’s quite complicated.
Here’s more detailed definitions:
- Here’s a Medicare Fact Sheet, something a little easier to read for the lay person.

- For chiropractic services, medically necessary means the patient must have “a significant health problem in the form of a neuromusculoskeletal condition necessitating treatment, and the manipulative services rendered must have a direct, therapeutic relationship to the patient’s condition and provide a reasonable expectation of recovery or improvement of function. The patient must have a subluxation of the spine, as demonstrated by x-ray or physical exam.”
- Treatment by means of manual manipulation of the spine to correct a subluxation (incomplete or partial dislocation of a joint or organ.[1] Wikipedia ) (that is, by use of the hands).
- Patient must require treatment by means of manual manipulation.
Manipulation services rendered must have direct therapeutic relationship to the patient’s condition.
There must be a reasonable expectation of recovery or improvement of function resulting from the planned treatment. CMS.gov * - Medicare Exclusions from Coverage
- Note that the specimen Medicare Advantage policy we used to analyze coverage has exclusions on page 115 for chiropractic, they only cover what Medicare covers, nothing extra!
- For those of you who think that “Medicare for All” will be the solution to every health problem and that Medicare pays everything, take a look at this NINE page bulletin on the the Medicare records required from your chiropractor.

- Sample Medicare Advantage Plan
- Use Ctrl F & Search adobe.com/searching-pdfs
- Sample Medi Gap EOC Plan G
- Medi Gap will provide coverage for the coinsurance amount or, in the case of hospital outpatient Services, the copayment amount of Medicare Eligible Expenses under Part B …, subject to the Medicare Part B Deductible provided the Subscriber is receiving concurrent benefits from Medicare for the same Services. Blue Shield EOC *
FAQ Chiropractor
- Does blue shield 65 plus cover any chiropractor care as basic Medicare does?
- How do I find a Chiropractor for the Inspire Plan?
.
- How do I find a Chiropractor for the Inspire Plan?
- Here’s our webpage on what Medicare offers for chiropractic. If you have further questions, please post in the ask a question section on that page. MAPD plans are required to offer at least as much coverage as Medicare does.
- See the summary of benefits for the Blue Shield plan you are interested.
- See link at top of page to enroll. No extra charge for our help.
- call ASH American Specialty Health Network customer service at (800) 678-9133
Do #Health Care Reform compliant plans cover chiropractic?
- No, Chiropractic is Excluded on page 106 of the Specimen policy, Page 14 brochure It’s not an essential benefit, in CA
- Here’s the CA Kaiser Benchmark Plan which is the “model” for ACA compliant plans
- Other States may cover chiropractic, but CA doesn’t. Here’s a report from dynamic chiropractic.com
- However,
- Blue Shield INDIVIDUAL
- Chiropractor benefits available for Silver 1950 PPO and Silver 2600 HDHP PPO plans as of Jan 1, 2021
- We are the first off-exchange health plan to offer embedded chiropractic services to members through the American Specialty Health (ASH) network with Silver 1950 PPO and Silver 2600 HDHP PPO plans.
- Benefits include:
- $15 copayments for Silver 1950 PPO
35% coinsurance for Silver 2600 HDHP PPO
Both plans have an annual limit of 15 visits
- Blue Shield INDIVIDUAL
At one time you could Buy your OWN Chiropractic Plan!
- But Landmark Health Plan has discontinued selling for individuals. Employer Groups can still enroll.
- Provider Directory
Physical Therapy, Ambulance, Cancer
#Physical therapy/occupational therapy/speech-language pathology services
- Medicare Part B (Medical Insurance) helps pay for medically necessary, see clinical guidelines!,
- outpatient physical medicare.gov/physical-therapy
- and Occupational therapy
- and. Speech-language pathology services
- Your medical record must include information to explain why the services are medically necessary
- A Medicare contractor like Livanta may review your medical records to be sure your therapy services were medically necessary. This happens when your bills go over say $2k cms.gov/theraphy caps
- Your therapist or therapy provider must give you a written notice before providing services that aren’t medically necessary. This includes therapy services that are generally covered but aren’t medically reasonable and necessary for you at the time.
- This notice is called an “Advance Beneficiary Notice of Noncoverage” (ABN). The ABN lets you choose whether or not you want the therapy services. If you choose to get the medically unnecessary services, you agree to pay for them.
Who’s eligible?
All people with Part B Out Patient are covered as long as the services are medically reasonable and necessary.
Your costs in Original Medicare
You pay 20% of the Medicare-approved amount, and the Part B deductible applies. If you have a Medi Gap or Medicare Advantage plan, those will pay all or part of the 20%.
Resources & Links
- The Best Quadriceps Exercises to Build Stronger Thighs Very Well.com
- Your Medicare Benefits Page 91
- Medicare & Home Health Care
- kindred health care.com your-guide-to-medicare-and-transitional-care
- torrance memorial.org/transitional-care/
- MLN Transitional Care Management Services pdf

- medicare.gov/transitional-care-management-services html
- 42 CFR § 410.60 – Outpatient physical therapy services: Conditions
- The complete Medicare guide for physical, occupational, and speech therapy.
- What does Medicare cover for outpatient rehabilitation therapy? Medicare Made Clear
- CMS.gov Physical Therapy – Home Health
- medicare.gov/physical-therapy-services
Medicare Coverage – #Ambulance # 11021
Resources & Links
- forbes.com/insurance-for-ambulance-rides/
- New California Law Offers Fresh Protection From Steep Ambulance Bills KFF.org – no balance billing – out of network
FAQ’s
- Question: Non-emergency ambulance transportation
. - Answer You may be able to get non-emergency ambulance transportation if you need it to treat or diagnose your health condition and the use of any other transportation method could endanger your health — Get the details on page 6 of the above publication, even MORE details Medicare Benefit Policy Manual Chapter 10 – Ambulance Services
#DROPPED HEAD SYNDROME
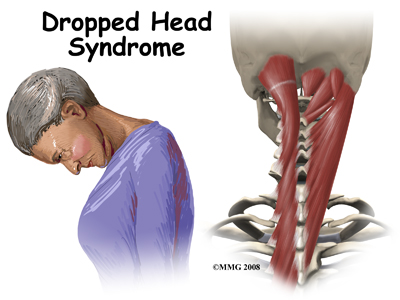
One of the extra things we do for our clients, friends & web visitors who post questions in the comments below, is extensive internet research. Here we go…
In addition to the physical therapy benefit in Medicare, Employer Group or Individual & Family plans, how about doing physical therapy at home, the gym and using silver sneakers?
- humpal physical therapy.com/Dropped-Head-Syndrome photo credit too
- spine-health.com/easy-chest-stretches-neck-pain
- mayfield clinic.com/neck stretches & strengthening
- Impact physical therapy
- Caring Medical.com




https://kffhealthnews.org/news/article/prosthetic-limbs-private-insurance-coverage-denials-amputees/
https://kffhealthnews.org/news/article/watch-why-insurance-companies-are-denying-coverage-for-prosthetic-limbs/
https://www.patientadvocate.org/connect-with-services/copay-relief/
https://www.justiceinaging.org/wp-content/uploads/2016/04/Durable-Medical-Equipment_The-Basics-for-California-Advocates.pdf
https://healthlaw.org/wp-content/uploads/2020/02/NHeLP-MediServicesGuide-Complete-Ch10.pdf
Financial Assistance Available to People Living with Diabetes Through New Co-Pay Relief Fund Supported by ADA | American Diabetes Association
Co-Pay Relief Program – Patient Advocate Foundation
Assistance and social programs | CA.gov
https://diabetes.org/newsroom/financial-assistance-available-to-people-living-with-diabetes-through-new-co-pay-relief-fund-supported-by-ADA
https://www.patientadvocate.org/connect-with-services/copay-relief/
https://www.ca.gov/topics/assistance/
https://healthlaw.org/wp-content/uploads/2020/02/NHeLP-MediServicesGuide-Complete-Ch10.pdf
https://www.justiceinaging.org/wp-content/uploads/2016/04/Durable-Medical-Equipment_The-Basics-for-California-Advocates.pdf
Will Medicare cover testing for Corona Virus?
Yes, under Part B. See Medicare.Gov for more details Maybe when the pandemic is over, NO?
Medicare Advantage Plans are mandated to cover A & B, so it will be covered by those too.
Medi Gap plans will pay the 20% co pay that Medicare doesn’t pay.
Coronavirus testing looks for signs of a coronavirus infection in nasal secretions, blood, or other body fluids. Coronaviruses are types of viruses that infect the respiratory system. They are found in both animals and people. Coronavirus infections in people are common throughout the world. They don’t usually cause serious illness.
Sometimes a coronavirus that infects animals will change and turn into a new coronavirus that can infect people. These coronaviruses can be more serious and sometimes lead to pneumonia. Pneumonia is a life-threatening condition in which fluid builds up in the lungs.
Three of these new coronaviruses have been discovered in recent years:
SARS (severe acute respiratory syndrome), a serious and sometimes fatal respiratory illness. It was first discovered in China in 2002 and spread around the world. An international effort helped quickly contain the spread of disease. There have been no new cases reported anywhere in world since 2004.
MERS (Middle East respiratory syndrome), a severe respiratory illness discovered in Saudi Arabia in 2012. The illness has spread to 27 countries. Only two cases have been reported in the United States. All cases have been linked to travel or residence in or around the Arabian Peninsula.
COVID-19 (coronavirus disease 2019). It was discovered in late 2019 in Wuhan City, in the Hubei Province of China. Most infections have occurred in China or are related to travel from Hubei Province. There have been some cases reported in United States. The outbreak is being closely monitored by the Centers for Disease Control (CDC) and the World Health Organization (WHO).
See our main page on Corona Virus and Insurance Coverage – Including Government Benefits
If I stay overnight in a hospital, doesn’t that make me an inpatient, so that I can then qualify for Skilled Nursing care, etc?
Am I an inpatient or outpatient?
Staying overnight in a hospital doesn’t always mean you’re an inpatient. Your doctor must order your hospital admission and the hospital must formally admit you for you to be inpatient. Without the formal inpatient admission, you’re still an outpatient, even if you stay overnight in a regular hospital bed, and/or you’re getting emergency department services, observation services, outpatient surgery, lab tests, or X-rays. You or a family member should always ask the hospital and/or your doctor if you’re an inpatient or an outpatient each day during your stay, since it affects what you pay and can affect whether you’ll qualify for Part A coverage in a skilled nursing facility.
A “Medicare Outpatient Observation Notice” (MOON) is a document that lets you know you’re an outpatient in a hospital or critical access hospital. You must receive this notice if you’re getting observation services as an outpatient for more than 24 hours. The MOON will tell you why you’re an outpatient receiving observation services, rather than an inpatient. It will also let you know how this may affect what you pay while in the hospital, and for care you get after leaving the hospital. Citation Medicare & You 10050 or Medicare Benefits 10116 See links above
Is the part b premium tax deductible?
Not that I’m aware of. Please check with competent tax or legal counsel. Here’s some links and information I do have.
Self Employed – Line 29 deduction of health Insurance Premiums
Savings from an HSA – Health Savings Account can be used to pay premiums – double check the rules and citations on our HSA webpage. See Publication 502 Medical & Dental Expenses
See the Kaiser Foundation Report on Part D & B premiums vs spending.