Uh Oh Oscar Individual IFP won't be renewing or selling in 2024!
California Cigna + Oscar Small Group will still be here
Oscar consistently had a 100% MLR Medical Loss Ratio. Modern Health Care * Meaning they paid out in claims, every nickel they took in, in premiums.
Resources & Link
Oscar announcement to brokers 5.9.2023
All our plans are Guaranteed Issue with No Pre X Clause
Quote & Subsidy #Calculation
There is No charge for our complementary services
Watch our 10 minute VIDEO
that explains everything about getting a quote
- Our Quote Engine Takes all the complexity out of using pencil and paper to figure out the premiums per the Obamacare/ACA rules under CFR §1.36B-3 *
- Get more detail on the Individual & Family Carriers available in CA
VIDEO Instructions on how to
#ENROLL ONLINE direct,
Quotes & Enroll Covered CA
Oscar’s Focus
Oscar’s Health Insurance focuses centers around the Internet and mobile applications. Another click and appointment options — a free doctor’s call or a visit to a primary care physician or specialist — are splashed on the screen with estimated costs. A consumer could expect to shell out a total of $200 in co-pays and typical prescriptions or tests for a visit to a specialist. Oscar offers an Exclusive Provider Organization plan, or EPO — a hybrid of the HMO and PPO models. Consumers, for example, receive no coverage out of network, but unlike an HMO they don’t need a primary care physician or a referral to see a specialist. Providence Health & Services, UCLA Health, St Joseph, HOAG, Huntington Memorial and USC Keck have signed on to Oscar’s network, giving it 19 hospitals and 11,000 MD’s in Los Angeles. Orange County has 9 hospitals and 5,000 providers.
All plans are EPOs with Doctor on Call, Concierge, and Step Rewards for staying active. Even better, Oscar never requires referrals to see a specialist. This means you don’t need to book an appointment with a primary care provider just to get a permission slip, saving you time and money.
Classic plans
Classic plans have higher monthly premiums and lower annual deductibles than Simple plans. Most plans provide pre-deductible copays for routine care and drugs. All plans have either coinsurance or affordable copays after you hit your deductible.
Saver plans
(Non Standard)
Saver plans are low premium, high deductible plans. In California, these are plans that work alongside a Health Savings Account (HSA). With HSA compatible Saver plans, you pay the full negotiated rate for care out of your HSA until your reach your deductible. After that, Oscar pays 100% for any covered care.
Oscar’s Simple Plans
(Non Standard)
offer something different, they combine the deductible and Out of Pocket Maximum as one number. The kicker, you still get pre-deductible benefits. For example, you have a $4,500 deductible and MOOP on the Gold Simple plan, however you can go to the doctor, get your labs and x-rays all at a flat co-pay prior to meeting your deductible. Simple!
In 2021 Oscar paid a lot of claims! Their MLR Medical Loss Ratio was 99.7% ! Modern Health Care * Yahoo * Covered CA * CMS.gov * Fierce Health Care *
Oscar 2023 Individual Brochure
Steve's VIDEO Introduction to this webpage and the Oscar Brochure
- No #Rando 's
- Oscar Billboard


- No Bozo's either
- Get OSCAR Quotes & Enroll ONLINE
- Appoint us as your Oscar Broker - No extra charge - 17 reasons why it's a good idea
VIDEO Instructions on how to
#ENROLL ONLINE direct,
Quotes & Enroll Covered CA
Oscar Pharmacy Rx Benefits
- Oscar Explanation of Coverage for #Rx
- What Pharmacies take Oscar Rx & Doctor Provider Finder
- Holistic alternative for erectile dysfunction to Viagra?
- See our FAQ section for more details on how Rx Coverage works.
Oscar #Member Portal Login
Links & Videos to help you get the most from Oscar
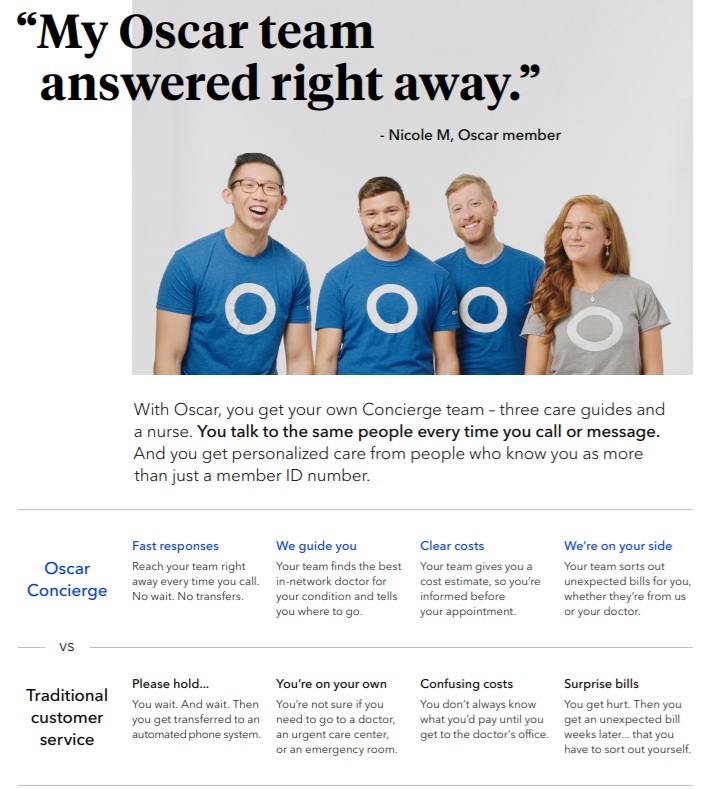
Concierge
Concierge – reinventing customer service with a personalized team of 3 care guides and a nurse – for every member.
- Oscar App Demo Video
- Two page summary of setting up an Oscar Account
- See why Oscar’s mobile app is the industry leader for member engagement.
- Doctor on Call Demo Video
- Concierge – We can help you get care VIDEO
- Oscar Care Guide VIDEO
- Making Health Care more human VIDEO
- How to find MD’s in Oscar App VIDEO
- Oscar Playlist 19 videos, about 15 seconds each VIDEO
- Modern Technology for Modern Care VIDEO
Every Oscar member gets a dedicated team of care guides and a nurse. See how it works.
- Concierge pdf
- Doctor on Call pdf
- Source – Oscar Broker Portal
- Our VIDEO explaining all the webpages below.
- Oscar Provider Finder
- hi oscar.com/concierge
- hi oscar.com/meet-oscars-concierge-teams
- hi oscar.com/care-team

Other links mentioned in our mini webinar:
#EPO vs HMO vs PPO?
EPO
All plans are EPOs Exclusive Provider Organization with Doctor on Call, Concierge, and Step Rewards for staying active. Even better, Oscar never requires referrals to see a specialist. This means you don’t need to book an appointment with a primary care provider just to get a permission slip, saving you time and money. See Page 5 of EOC Evidence of Coverage for more details.
Choice of Physicians and Providers
This is an Exclusive Provider Organization (“EPO”) plan.
Services must be performed or supplies furnished by an In-Network Provider in order for benefits to be payable. Typically, there are no Benefits provided when using an Out-of-Network Provider and You may be responsible for the total amount billed by an Out-of-Network Provider. The only exceptions are:
● Services received by an Out-of-Network Provider as a result of a medical Emergency, Urgent Care Visit, or an Authorized Referral as defined in the
DEFINITIONS section; and
● Covered Services received at an In-Network Facility, at which, or as a result of which, the Member receives Covered Services from and Out-of-Network Provider. Authorized Referrals and Covered Services received under the second exception are provided at In-Network Cost Sharing.
To maximize Your benefits, be sure to confirm that the Provider (e.g. a Physician or Hospital) You wish to see is an In-Network Hospital or an In-Network Provider (for Providers other than Hospitals) under Your Plan. Services must be performed or supplies furnished by an In-Network Provider in order for benefits to be payable, unless one of the exceptions listed above apply. 2020 EOC *
#TeleMed
This is our "Main Module" on Telemed. Not just one specific Company but Telemed for ALL companies, in general.
- Telehealth has quickly become one of our nation’s most essential health care services — a safe and low-cost way to access care.
- Millions of users have now experienced and embraced what telehealth has to offer. Many won’t go back to traditional ways of getting care, including your employees. To meet the evolving preferences of your workforce, you should offer a health plan with connected virtual care options. Learn More: Kaiser *
- Oscar covers Medically Necessary Covered Services offered through Telehealth by an In Network Provider subject to the terms and conditions of the their contracts with In Network Providers. Telehealth Visits from certain Oscar-designated Telehealth Providers are covered in full.
- Telehealth Visits can be requested through Oscar’s website, mobile application, and their customer service line 1-855-672-2755.
- Health Net Teladoc Medicare
- Teladoc (Telehealth) Introductory Flyer
- Teladoc (Telehealth) FAQs
- Teladoc (Telehealth) FAQs – En Español
- Teladoc Caregiver flyer
- Teladoc Caregiver FAQs
- hioscar.com/doctor-on-call
- Doctor On Demand.com
- hioscar.com/need-medical-advice-call-a-doctor-instead-of-your-mom
- EOC – Evidence of Coverage.
- Tele Med VIDEO Oscar
- OSCAR Tele Med 1 page flyer
- My CPA’s thoughts & research on Telehealth
- U.S. saw significant drop in telehealth use last year after rapid growth in 2020 Modern Health Care *
- Telehealth Companies Want Congress to Make Pandemic Expansion of Their Services Permanent Time Magazine 4.2022 *
- FAQs on Medicare Coverage of Telehealth
- Dental Visits Tele Health
Further clarification from Oscar:
- Our Doctor on Call benefit is on all Oscar plans and include Oscar physicians that are board certified in your state.
- These physicians are not specialists, they generally are listed as Internal Medicine, Primary Care, etc.
- These doctors are not found on our website because there is no way to visit/select which doctor you speak to.
- The physicians often service multiple states, as they are generally certified in multiple.
- Personally, when I used the Doctor on Call benefit (at 11 pm) the doctor called me within 10 minutes.
- If I called again today I would likely be speaking to a different physician.
- I checked with Oscar circa 4.4.2019 and their Tel Med is just for an initial visit. Check our Coronavirus page for updates on that.
- doctor on demand.com
- Emotional support helpline: 1-866-342-6892 – Optum
- AB 744 - TeleHealth
- AB 744 will require contracts issued, amended or renewed after January 1, 2021 between a health care service plan and a health care provider to specify that the provider who delivers services appropriately through telehealth be reimbursed on the same basis and to the same extent that the plan would have had the same service been provided in-person. The health plan cannot require the use of telehealth if the health care provider has determined that it is not appropriate nor does it limit the ability of the health plan and provider to negotiate the rate of reimbursement for a service. TeleHealth Resources.org *
- LA Times on Tele Med 8.2018
-
telehealth is the use of electronic information and telecommunications technologies to support long-distance clinical health care, patient and professional health-related education, public health and health administration. Technologies include videoconferencing, the internet, store-and-forward imaging, streaming media, and terrestrial and wireless communications.
-
Telehealth is different from telemedicine because it refers to a broader scope of remote healthcare services than telemedicine. While telemedicine refers specifically to remote clinical services, telehealth can refer to remote non-clinical services, such as provider training, administrative meetings, and continuing medical education, in addition to clinical services.
- AMA outlines key steps for advancing telehealth equity
- Telehealth didn't lead to unnecessary care in 2020, study says
- I checked with Oscar and their Tel Med is just for an initial visit.
- Here's what I googled for online therapists. Check with them and ask what Insurance Plans they take. Then double check on the official Insurance Company provider list.
#Why Oscar?
- The Uber of Health Care?
- Oscar Website
- Wikepedia on Oscar
- financials
- deepdive
- Oscar Health CEO: The days of high valuations are over Modern Health 5.17.2022
- Better Business Bureau Complaints
- 5 keys to success from the CEO of $3.2 billion healthcare start-up Oscar
- linkedin.com/mario-schlosser
OSCAR Rx & Doctor #Provider Finder
- Oscar Rx
- Oscar Rx FAQ's
- Oscar Network Options
- #Choice (formerly Circle) & Select
- Los Angeles 2022 * San Francisco
- Choice includes UCLA, UC Irvine & Cedars
- Oscar Network Search Instructions








https://www.hioscar.com/es/asset/broker-digital-toolkit
https://www.healthcarefinancenews.com/news/oscar-health-and-bright-health-are-curbing-ma-expansion-now
https://mhealthintelligence.com/news/hhs-issues-fraud-alert-to-caution-providers-against-telehealth-cons
https://californiahealthline.org/news/article/digital-mental-health-companies-scrutiny-concerns/
https://finance.yahoo.com/news/5-trends-pointing-telehealth-supplement-150000213.html
Hi, Steve.
Thanks, I’m all set with Oscar. I received a welcome letter and found instructions on making a web payment for my EPO 87 plan for Jan 1, 2018.
I also set up the auto-pay recurring payments as well.
Thanks for your help with the ACA insurance stuff here. Bye bye to Blue Shield of Calif. Their rates for the same PPO enhanced silver insurance were ridiculous.
Oscar is a newer, startup company, so the competition for business is exactly what President Obama and Congress intended when they set up the ACA, among many other patient protections for those of us with pre-existing conditions.
Thank you again,