Does Medicare Cover Skilled Nursing Facility (SNF) Care?
Medicare does cover skilled nursing facility (SNF) care — but only for a limited time and only if specific medical conditions are met.
This is not long-term care or permanent nursing home coverage.
In most cases, Medicare pays for short-term rehabilitation after a hospital stay, such as recovery from surgery, illness, or injury.
When Does Medicare Cover Skilled Nursing?
Medicare Part A may cover care in a Medicare-certified skilled nursing facility if all of the following apply:
- You had a qualifying hospital stay (at least 3 days inpatient)
- You need daily skilled care (such as physical therapy, IV medications, or wound care)
- You enter the facility within a short time after hospital discharge
- The care is ordered by a doctor and provided by licensed professionals
How Much Does Medicare Pay?
Medicare covers SNF care in stages:
- Days 1–20: Medicare pays 100%
- Days 21–100: You pay a daily copayment
- After Day 100: Medicare pays nothing
After 100 days, patients are responsible for all costs unless they have other coverage such as Medi-Cal or long-term care insurance.
What Medicare Does NOT Cover
Medicare does not cover:
- Long-term or permanent nursing home care
- Custodial care (help with bathing, dressing, eating)
- Care when skilled services are no longer needed
- “Medicare is designed for **short-term medical recovery — not long-term care planning.”
This is one of the most common misunderstandings — many people assume Medicare will pay for extended nursing home stays, but it generally does not.
Need help understanding your options?
✔ Compare Medicare Supplement plans
✔ Review long-term care alternatives
✔ Get help planning ahead before a health event
Start Here: What Type of Care Do You Need?
- Recovering after a hospital stay? → Skilled Nursing Facility (this page)
- Need care at home? → Medicare Home Health Care
- Need long-term help with daily living? → Long-Term Care Options
Find a Nursing Home - Medicare.Gov
- Find & compare nursing homes, hospitals & other providers near you Medicare.Gov
- Learn more about providers
CMS Guide to Choosing a #Nursing Home 02174
- Nursing Home Definitions Page 67
- Our Webpage on Long Term Care
- Finding a nursing home
- How to choose a nursing home - VIDEO
- More resources to finding home health & nursing homes
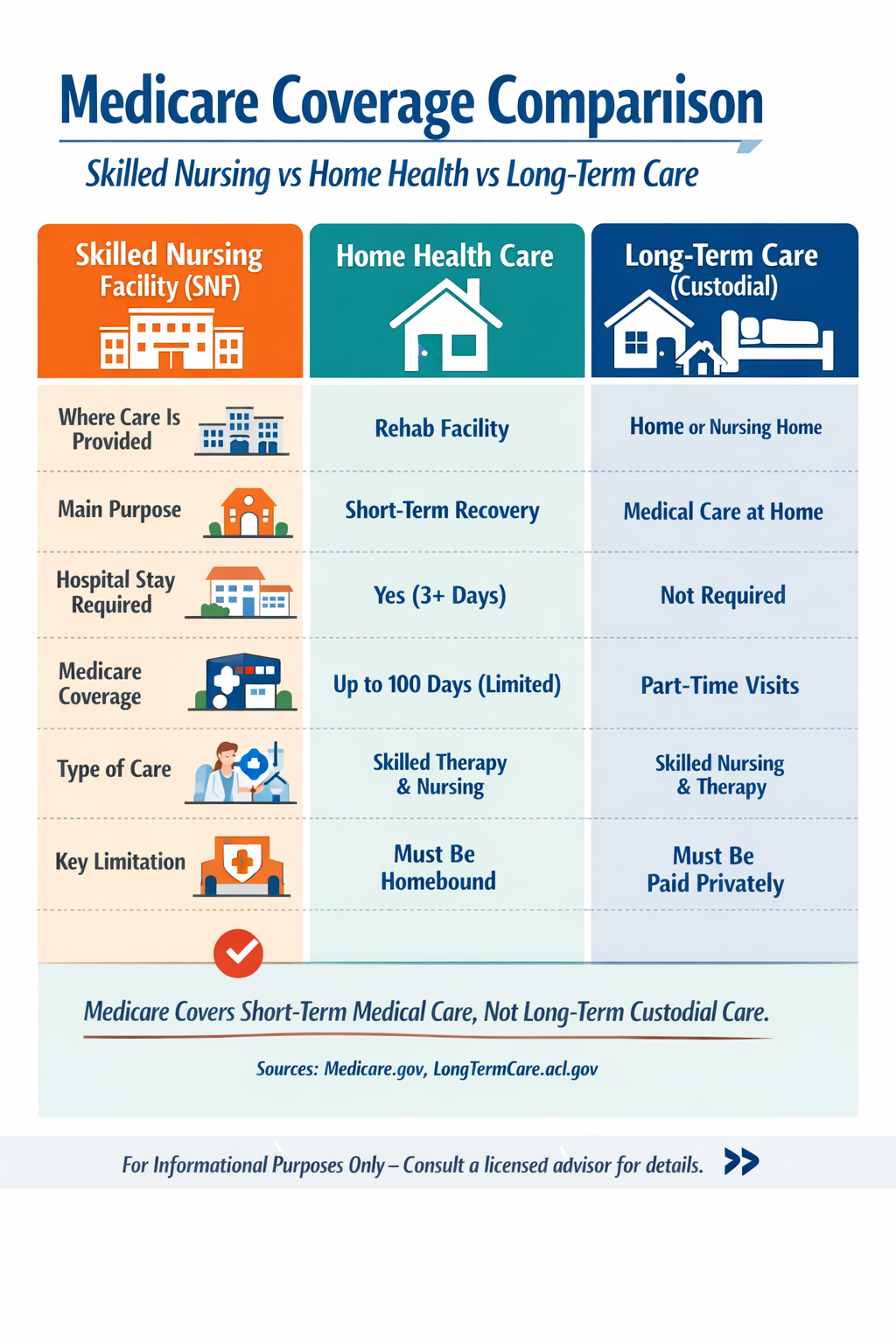
Medicare Coverage Comparison: Skilled Nursing vs Home Health vs Long-Term Care
| Type of Care | Skilled Nursing Facility (SNF) | Home Health Care | Long-Term Care (Custodial) |
|---|---|---|---|
| Where Care is Provided | Nursing facility / rehab center | Your home | Home, assisted living, or nursing home |
| Main Purpose | Short-term recovery after hospital stay | Medical care at home (nurse or therapy) | Help with daily living over time |
| Requires Hospital Stay? | Yes (typically 3+ inpatient days) | No (in many cases) | No |
| Type of Care | Skilled (therapy, IV meds, wound care) | Skilled (nurse visits, therapy) | Custodial (bathing, dressing, eating) |
| Medicare Coverage | Days 1–20: 100% Days 21–100: Copay After 100: Not covered |
Usually covered if medically necessary and homebound | Not covered by Medicare |
| Length of Coverage | Up to 100 days per benefit period | Intermittent / part-time visits | Ongoing / long-term |
| Key Limitation | Stops when skilled care is no longer needed | Must meet “homebound” and medical criteria | Must be paid out-of-pocket or insured |
| Common Misunderstanding | People think it covers long-term stays | People think it includes full-time caregivers | People think Medicare will pay — it won’t |
Bottom line: Medicare is designed for short-term medical care, not long-term living assistance.
Not sure which type of care applies to your situation?
✔ Get help understanding Medicare coverage
✔ Review long-term care planning options
✔ Compare Medicare Supplement plans
How Assisted Living Fits in the Care Continuum chcf 8/2024

- What is Assisted Living Opportunities to Advance Community-Based Care for Medi-Cal Enrollees CHCF 8/2024
How does Medicare pay for #SkilledNursing Homes - 10153 11359
Our Introductory You Tube VIDEO based on this manual
- Your costs for Skilled Nursing in Original Medicare You pay:
-
Days 1–20: $0 for each benefit period .
- Days 21–100: $194.50 coinsurance per day of each benefit period.
-
Days 101 and beyond: All costs. Medicare.gov *
-
- Clinical Guidelines explain the coverage so much better and in logical order!
- The two-midnight rule and Medicare Advantage: 7 updates Beckers Payer.com 2/2024
- Medi Cal Payments Fall Far Short of Covering Care Costs at Nursing Homes Skilled Nursing News.com 11/2024
- Medicare's VIDEO Nursing Home / Long-Term Care
- Planning for Discharge from a Health Care Setting VIDEO
- Long Term #Acute Care Publication # 11347
- Differences between Skilled Nursing, Long Term Acute Care & Inpatient Rehabilitation Facility
- Our FAQ on Sub Acute Care
- Find & compare nursing homes, hospitals & other providers near you Medicare.Gov
- Learn more about providers
- Calculate Cost of Long Term Care in your Area Genworth
- "Hospital at Home" Programs Improve Outcomes, Lower Costs But Face Resistance from Providers and Payers
- Pro Seniors Medicare & Skilled Nursing
- Medicare doesn't pay for:
- Our Webpagse on Long Term Care
Skilled nursing facility care
Medicare covers semi-private rooms, meals, skilled nursing and rehabilitative services, and other medically necessary services
(Clinical Guidelines – Oscar – Explains Medical Necessity Requirements so much better and in logical order!)
and supplies furnished in a skilled nursing facility after a 3-day minimum, medically necessary, inpatient hospital stay Medicare Policy Manual * Publication 10153 SNF * for a related illness or injury. An inpatient hospital stay begins the day the hospital formally admits you as an inpatient based on a doctor’s order and doesn’t include the day you’re discharged. You may get coverage of skilled nursing care or skilled therapy care if it’s necessary to help improve or maintain your current condition.
A SNF is a care center where nurses and nursing assistants are available to provide twenty-four hour care for patients to assist them with conditions in their transition between the hospital and a lower level of care such as the home. A SNF may also provide rehabilitation in order to improve the member’s function and decrease the burden of care. Oscar Clinical Bulletin *
To qualify for skilled nursing facility care coverage, your doctor must certify that you need daily skilled care (like intravenous injections or physical therapy) which, as a practical matter, can only be provided in a skilled nursing facility if you’re an inpatient.
You pay:
- Nothing for the first 20 days of each benefit period
- $185 Coinsurance per day for days 21–100 of each benefit period
- Sample Medicare Advantage Copay
- Medicare Advantage must pay at least as well and same qualifications as Original Medicare.
- MAPD can’t do “funny stuff” or they can get busted for Risk Adjustment Fraud
- Sample Medi Gap
- All costs for each day after day 100 in a benefit period Medicare.Gov SNF *
Medicare doesn’t cover long-term care or custodial care.
Medical Requirements
The beneficiary needs daily skilled care or rehabilitation services as ordered by a physician. These skilled services can only be rendered by, or under the direct supervision of, skilled nursing or rehabilitation staff. In addition, the skilled services the patient receives must be for a medical condition they were treated for during the three-day qualifying hospital stay, or for a condition that arose during that hospital stay or while the patient was receiving Medicare-covered SNF care.
The requirement of “daily” skilled services should not be taken so literally that occasional sessions missed due to holidays or illness will make the patient not meet the daily requirement for skilled services.
See Oscar’s Clinical Guidelines – It’s explained so much better!
Daily Skilled Services Defined
Skilled nursing services or skilled rehabilitation services (or a combination of these services) must be needed and provided on a “daily basis,” i.e., on essentially a 7-days-a week basis. A patient whose inpatient stay is based solely on the need for skilled rehabilitation services would meet the “daily basis” requirement when they need and receive those services on at least 5 days a week. (If therapy services are provided less than 5 days a week, the “daily” requirement would not be met.) Medicare Benefits Policy Manual SNF Services
Links & Resources
- True Freedom Home Health Plan – Enroll BEFORE you need it.
- Nolo on Inpatient Stays
- Appeal when a hospital changes your status from “inpatient” to “outpatient getting observation services” Medicare.gov
CA Dept of Aging – Home & Long Term Care Booklet
Please note, there are updates all the time, double check everything.
#Taking Care of Tomorrow Booklet
NAIC Shoppers Guide to Long Term Care





https://www.ccld.dss.ca.gov/carefacilitysearch/
https://bellmedex.com/medicare-daily-rates-for-skilled-nursing-facilities/
https://www.kindredhospitals.com/locations/california/help-paying-your-bill
https://individuals.healthreformquotes.com/covered-ca-introduction/magi/income-chart/
https://www.kindredhospitals.com/news-stories/research-and-insights
https://kffhealthnews.org/news/article/long-term-care-nursing-homes-medicare-ai-prior-authorization/