Already Know Your Medi-Cal Share of Cost?
If your county worker or BenefitsCal notice has already told you your monthly Share of Cost amount, the next step is finding qualifying health expenses that may help reduce it — sometimes even to $0.
Many people use dental insurance premiums, Medicare Supplement premiums, vision coverage, or other recurring medical expenses to offset their Share of Cost and qualify for full Medi-Cal benefits sooner.
Start Here: Lower or Eliminate Your Medi-Cal Share of Cost
If Medi-Cal says you have a monthly Share of Cost, you may be able to reduce it — sometimes even to zero — by using certain recurring health expenses, such as dental insurance, vision coverage, Medicare Supplement premiums, or other medical expenses. The first step is figuring out your target amount, then matching it to expenses that may count.
Not sure where to begin? Most people should start with the Share of Cost calculator. If you already know your monthly amount, you can jump directly to dental plan options or email Steve for a free review.
What This Page Helps You Do
- Estimate your Share of Cost before shopping for any plan.
- Learn which health expenses may count toward reducing your Share of Cost.
- Find dental or other recurring expenses that may help offset the monthly amount.
- Get proof of coverage that may be submitted to the county or through BenefitsCal.
- Review related IHSS, Medi-Cal, and Medi-Gap issues if your situation is more complicated.
Quick Links
Need to know what expenses may count?
Visit the eligible medical expenses page.
Need to upload proof to the county?
See how to upload documents to BenefitsCal.
Trying to fix a past month?
Review how to fix Medi-Cal Share of Cost retroactively.
Trying to qualify for IHSS?
Visit the IHSS and Share of Cost page.
On Medicare?
See how a Medi-Gap premium may help lower Share of Cost.
Important: Steve Shorr is a California health insurance agent, not an attorney, tax adviser, county worker, or Medi-Cal eligibility worker. This page is for general information and practical insurance guidance. Each county case may be different.
Start Here to lower your Medi-Cal Share of Cost to $0
Step 1: Estimate Your Share of Cost
Not sure what your Share of Cost should be? Start with the estimate first. That will give you a target amount to work with.
Step 2: Already Know Your Share of Cost?
If you already know the monthly amount, the next question is finding a qualify dental plan and premium or other recurring health expense to offset it. The AmFirst plan provides proof of coverage for Medi Cal within 24 hours! Scroll down for sample letter.
Step 3: Gather Proof of Expenses
To use health expenses rather than purchasing dental, Medi Gap, etc. properly, you may need records such as premium invoices, receipts, policy documents, or proof of payment.
Step 4: Need Help Choosing a Plan?
If you want help reviewing dental plan options or figuring out whether a plan premium could help lower your Share of Cost, we can help you review your options.
How This Strategy May Work
- Medi-Cal may allow Health Insurance like, dental, vision and Medi Gap and certain health expenses to be applied toward the monthly Share of Cost. Scroll down for details & citations.
- For some people, a dental insurance premium is one of the most practical recurring expenses to consider.
- If the monthly expense is large enough, it may reduce the Share of Cost significantly or even to zero. Use our calculator.
- Each situation is different, so it helps to estimate the amount first and then compare plan costs. Most often your Social Worker will tell you how much you need to spend.
FAQ’s
What is a Medi-Cal Share of Cost?
It is the amount of medical expenses you may have to incur in a month before Medi-Cal begins paying.
Can dental insurance help reduce Share of Cost?
In some situations, yes. A dental plan premium may count as an allowable health expense that helps reduce the amount.
Do I need to know my exact Share of Cost first?
It helps. If you do not know the amount, start with the calculator or worksheet first.
Is this legitimate?
Many people are understandably skeptical the first time they hear that certain insurance premiums may help reduce a Medi-Cal Share of Cost. In some situations, health insurance premiums may count as allowable medical expenses under Medi-Cal rules. Learn More Center for Health Care Rights
You are purchasing a real insurance policy from a licensed company or association, not paying a fee for a “secret program” or loophole. AmFirst Insurance Delta Blue Shield etc. Proof of coverage documents are generally available after enrollment, scroll down for sample and those documents may then be submitted to the county – Benefits Cal for review.
Every county case is different, and approval is not guaranteed. County workers may ask for additional proof, including premium invoices or payment confirmation. Always verify your specific situation with your county worker.
Steve Shorr is a licensed California insurance agent who has specialized in health insurance since 1975. He has hundreds of unsolicited testimonials
What if I want the detailed rules and citations?
Use the technical resources below. The main purpose of this page is to help you move to the next step quickly.
Technical and Research Resources
- Aged and Disabled Medi-Cal Resources
- Income and change reporting resources
- MAGI income category guides
- “How to Eliminate Medi-Cal Share of Cost with the 250% Working Disabled Program”
- Calculate Instantly Medi Cal Share of Cost and Zero it out!
- FAQ’s Share of Cost
- How to upload documents to BenefitsCal.com
- How to use medical expenses to lower share of cost
- IHSS In Home Supportive Services
- Medi Gap to lower share of cost Medi Cal IHSS
- Redetermination Medi Cal Share of Cost
Take the Next Step
Estimate your Share of Cost, compare dental plans, or contact Steve for help reviewing your options.
| Estimate Share of Cost | View Dental Plans | Email Steve |
This page is for general educational purposes only and is not legal advice. Medi-Cal rules, county administration, and acceptable proof may vary by circumstance.
Sample Proof of Dental Insurance for Uploading to BenefitsCal.com
View and fill out enrollment application

|
Hi Steve, Good Morning! Medi-Cal reviewed my Mom’s case and eliminated her share of cost effective as of February 1. My family is very grateful that this issue was resolved in a very timely manner. Thank you very much again for your assistance in facilitating this effort. I will definitely keep your contact information for any future insurance needs. Sincerely, Don V
****************** Thank you so much. Eliminating her share of cost will allow her to stay living at our home longer so it’s very wonderful. Mary
Hi Steve, THANK YOU SO MUCH for getting back with me. You are a wealth of knowledge and I am so grateful to connect with you Thank you! Carie C
|
Child Sub Pages

Lower Your Medi-Cal Share of Cost — How It Works
If you have a Medi-Cal Share of Cost, you may be able to reduce it to $0 legally by using health insurance premiums strategically.
This generally applies if your income is too high to qualify for $0 Share of Cost, and you are currently paying anywhere from $100 to $2,000 or more per month before coverage begins.
The idea is simple: Medi-Cal may allow certain health insurance premiums and medical expenses to be deducted when determining your Share of Cost. By choosing the right combination of plans, it may be possible to reduce your Share of Cost significantly — or even to $0.
Example
Monthly Share of Cost: $1,200
Dental + Insurance Premiums: $500
Result: Share of Cost reduced to $0
Every situation is different. Some people use dental insurance, Medicare A & B, Medi Gap premiums, or other qualifying plans as part of the strategy. The key is choosing the right approach based on your specific situation.
If you want me to review your situation, send me your Share of Cost amount and, if you have it, your Medi-Cal Notice of Action. I will take a look and let you know what your options are.
Email Your Share of Cost for a Free Review
 AmFirst Insurance Company Dental Coverage Application with premiums up to $425
AmFirst Insurance Company Dental Coverage Application with premiums up to $425
You can also use our Share of Cost worksheet and calculator to estimate your situation.
Do you need to lower your share of cost by more than $425 in premiums?
Get more dental coverage
Dental For #Everyone,
More detail & Information on Enrolling in the AmFirst Plan
- Need to spend more than $310 – up to $435??
- Scroll down to learn about Medi Gap, Part D, etc.
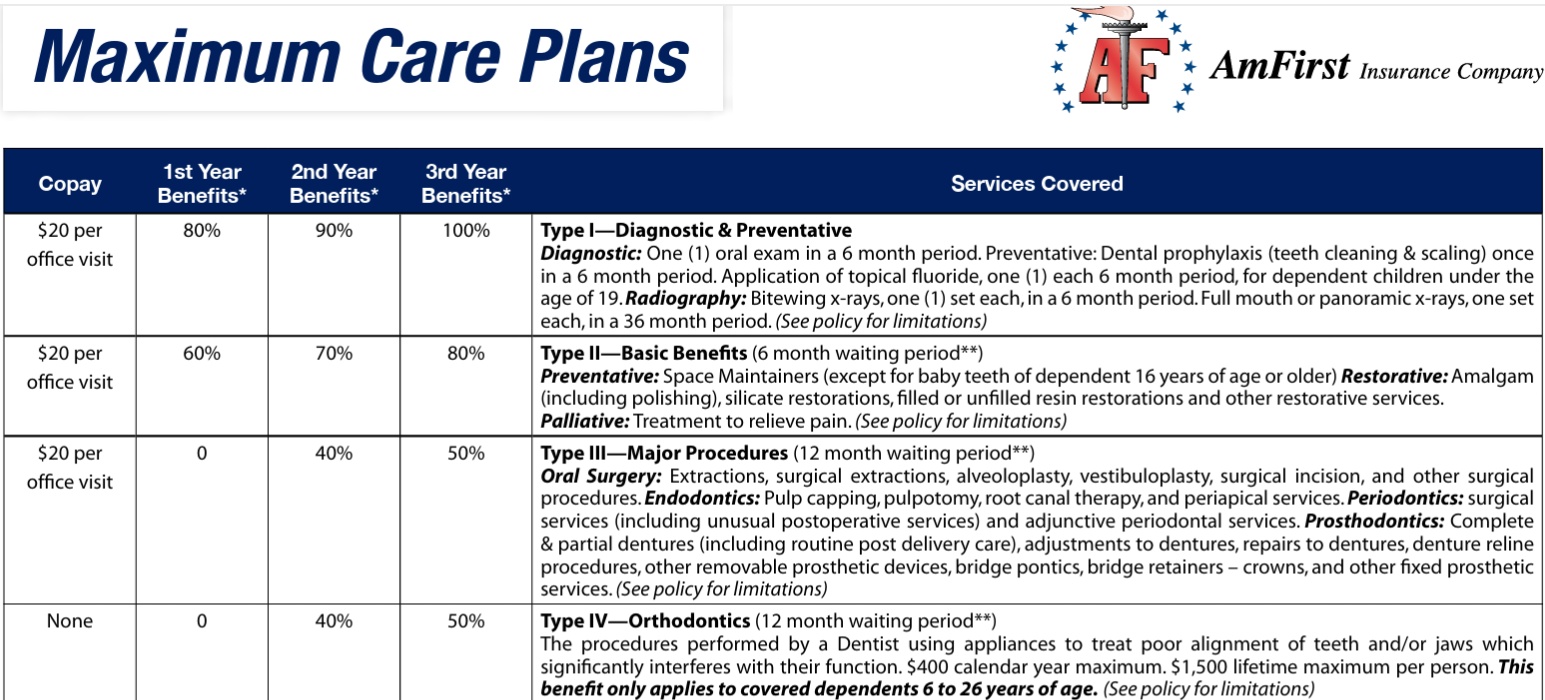
- Special Plan for Share of Cost – Maximum Care Plans
- Maximum Care Plans Summary of Benefits
- Plus Plan
- If you need to spend more for Share of Cost – Check out the Dental Plus Plan
- You get proof of coverage to upload to Benefits Cal.com the next day!
- Enrollment Form Plus & Maximum Care Plans
- Just fill out the form, take a picture and email to us at [email protected]
- There is no charge for our expertise in helping you. We get paid by the Insurance Company.
- Receipt and proof issued within 24 working hours
- AI summary of proofs needed by Medi Cal
- Submit proof of your health insurance premiums to the county Medi-Cal office
- Effective date only the 1st of the month, but can be BACKDATED as far back as the last day of the month.
- Email us [email protected] and check this webpage, we may be able to go back several months!
- Client – Member Portal
- Just fill out the form, take a picture and email to us at [email protected]
- Use ANY Dentist – UCR Usual Reasonable & Customary
- Certificate of Coverage EOC
- travel and fitness.org dues are included in the premium
- You should get approval and your policy in a day or two. Then just upload (get instructions) to BenefitsCal.com
- How to upload documents to BenefitsCal.com
- How to use medical expenses to lower share of cost
- Share of Cost FAQ’s
Can Lowering Your Share of Cost Also Help You Change Medicare Advantage Plans or Get Medi Gap?
If you have Medicare and Medi-Cal with a Share of Cost, reducing that Share of Cost may do more than just lower your medical expenses.
It may also create opportunities to change your Medicare Advantage plan outside of the normal enrollment periods.
How It Works
- If your Medi-Cal becomes active (your Share of Cost is met), your eligibility status may change
- Changes in Medicaid (Medi-Cal) status can trigger a Special Enrollment Period (SEP)
- This may allow you to switch plans without waiting for Open Enrollment
Important for 2025 and Beyond
- The old “once per quarter” rule for dual-eligible beneficiaries has been discontinued
- Plan changes are now generally tied to changes in your Medicaid eligibility or specific plan options
- Not all plan changes are available year-round
Bottom line: If your Share of Cost changes or is eliminated, you may qualify for additional Medicare plan options.
Quick Check
- Do you have Medicare Part A & B?
- Do you have Medi-Cal (even with Share of Cost)?
- Has your Share of Cost recently changed or been met?
- More —-
- Approx. income?
- ZIP code
- MAPD Plan you have now?
- Date of Birth
If YES → You may qualify for a Special Enrollment Period.
Dental For #Everyone,
has an excellent website with full brochures, Instant online quoting and enrollment
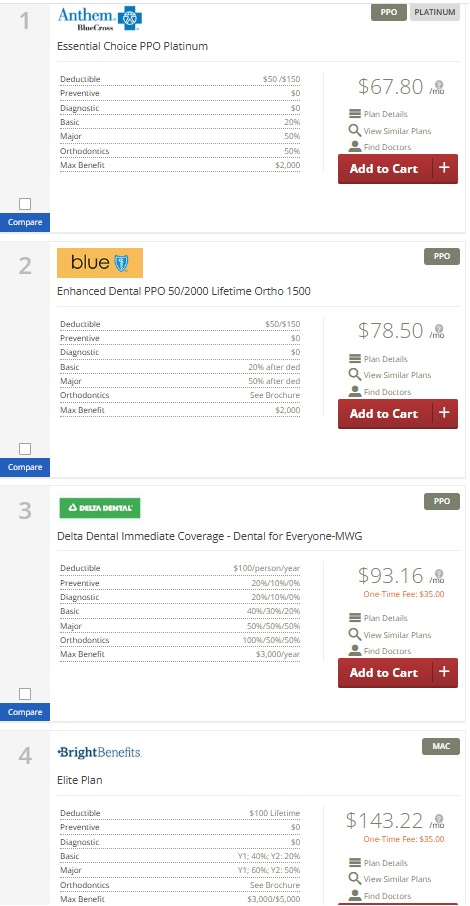
- Dental for Everyone includes quotes from
- Careington Discount Plan
- Bright Benefits
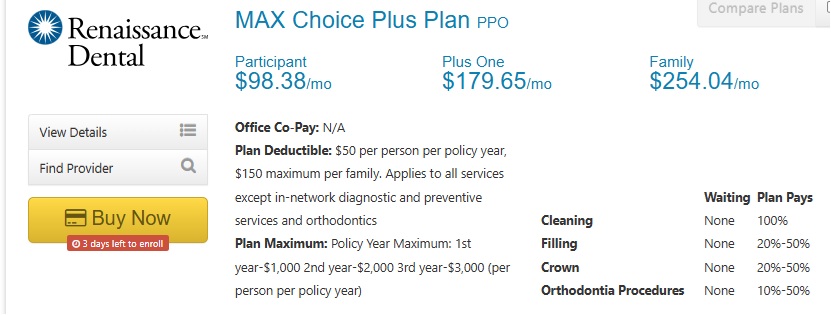
- Renaissance Dental
- Delta Dental
- AmFirst - but not the special one for share of cost with premium to $425
- One of our colleagues on how Dental for Everyone Works.
- Some of our webpages on dental
- VSP Vision
- The AmFirst is our most popular plan for those who need to buy health insurance to lower their income for Medi Cal Share of cost!
- Plans are available from $85 up to $425/month
- Application – Just fill it out, check off the premium you need, take a picture and email [email protected] to us
- Proof of coverage for upload to BenefitsCal.com is issued often the same day!
Ways to lower your Medi-Cal #Share of Cost
If you don’t have Full Scope Medi Cal
Get a Vision, Dental or Medi Gap Policy
You can Avoid a Share of Cost dpss flyer in the (ABD-MN) Aged, Blind and Disabled our webpage – Medically #Needy Program (CANHR Fact Sheet 8.14.2023) (My highlighted version) program and then qualify for no-cost Medi Cal A & D FPL.
Just purchase Health Insurance California Code of Regulations 22 ccr 50555.2 : CA Insurance Code §106 or show Medical Expenses..
- dental or vision insurance get quotes Dental For #Everyone, * Quotit.
- Special Plan for Share of Cost – Maximum Care Plans
- You can get several dental and vision policies. This kind of makes sense as there isn’t a COB Co Ordination of Benefits Clause on Individual Plans, so you could possibly collect more than the actual claim
- Medi-Gap
- Note that if you have Kaiser or another Medicare Advantage Program, you can’t get Medi Gap
- We are NOT telling you to cancel your MAPD program, but you might want to consider it.
- MAPD vs Lower Share of Cost?
- SEP’s Special Enrollment Periods to drop MAPD if Medi Medi any quarter Medicare.gov
- MAPD options for Dual Eligibles Medi Cal and Medicare
- GET QUOTES & ENROLL Medi Gap Quotit *
- Contact us [email protected] if you want quotes from UnitedHealthcare
- Note that if you have Kaiser or another Medicare Advantage Program, you can’t get Medi Gap
- Part B Medicare
- Part D Rx,
- Do you have this in your Medicare Advantage Program?
- Medical Expenses, including Adult Diapers – our webpage
- Covered CA if you are under 65? Get quotes
- Email us [email protected] every situation is different, we will need to research if this will work for you.
“Tell me your monthly Share of Cost amount or how much your Social Worker at Medi Cal said you need to spend on premiums and I’ll tell you exactly how much insurance you need.”
Add a section:
✅ This strategy is permitted under California Medi-Cal rules
✅ Premium payments are allowable medical deductions
✅ No income manipulation required
✅ No assets moved
Also add:
By submitting the information below , you are agreeing to be contacted by Steve Shorr a Licensed Sales Agent by email, texting or Zoom to discuss Medicare or other Insurance Plans as relevant to your inquiry. This is a solicitation for Insurance
Need to spend more $$$ to get to Zero Share of Cost?
We have additional Dental, Vision & Medi Gap plans
Dental For #Everyone,
has an excellent website with full brochures, Instant online quoting and enrollment
- Dental for Everyone includes quotes from
- Careington Discount Plan
- Bright Benefits
- Renaissance Dental
- Delta Dental
- AmFirst - but not the special one for share of cost with premium to $425
- One of our colleagues on how Dental for Everyone Works.
- Some of our webpages on dental
- VSP Vision
By submitting the information below , you are agreeing to be contacted by Steve Shorr a Licensed Sales Agent by email, texting or Zoom to discuss Medicare or other Insurance Plans as relevant to your inquiry. This is a solicitation for Insurance
General Information on Share of Cost
Center for Health Care Rights.com 

- There are 2 ways to reduce or eliminate the Medi-Cal Share of Cost:
- 2. Buy health insurance each month to get rid of the monthly Medi-Cal Share of Cost.
- ► The money you spend on health insurance premiums each month will reduce your income so that you meet the Medi-Cal monthly income limits of $1,801 for a single person or $2,433 for a married couple.
- ► Example: If you are over the income limit by $50, you can buy a dental policy that costs $50 a month.
- ► Any health insurance premiums can be used to eliminate the Medi-Cal Share of Cost. For example:
- ► Dental or vision insurance;
- ► Medicare Part D drug plan;
- ► Medigap Insurance (private insurance policies that pay Medicare copayments and deductibles).
- ► Your Medi-Cal Social Worker can tell you how much you need to spend on health insurance to get rid of the Medi-Cal Share of Cost.
- Send proof of the extra health insurance to Medi-Cal
- ► Provide Medi-Cal office with written proof that you are buying health insurance on a monthly basis to eliminate the Medi-Cal Share of Cost. Medi-Cal office will update your Medi-Cal record to show that you have full Medi-Cal with no Share of Cost.

- See My Medi Cal information

- 2. Buy health insurance each month to get rid of the monthly Medi-Cal Share of Cost.
More explanation of how share of cost works and ways to eliminate it – bring it to ZERO!
Who pays Medicare Part B you or Medi Cal?
Medicare Savings Programs & LIS Low Income Subsidy aka Extra Help
If you pay, it lowers your Share of Cost!
We can help you enroll in Medicare Part B Out patient, Doctor Visit and Part D Rx
Visit our Webpage on how to lower costs using
unreimbursed Medical Expenses
More explanation, details & Faq’s
Explanation of Share of Cost #SOC
- If your monthly income is higher than the limits to qualify for SSI or the A&D FPL program, but you meet the criteria of the low asset-level requirements, you may still qualify and be eligible for Medi-Cal with a share of cost (SOC).
- Uh Oh 2026 it looks like there is an asset test! Learn More Insure Me Kevin.com * Daily News * CANHR Fact Sheet * CANHR FAQ’s *
- SOC functions like a deductible, it’s not a percentage, like a Co-Pay. You must pay this amount in any month you incur medical costs. After your SOC is paid, Medi-Cal will pay the remaining amount of your medical bills for that month.
- Note: A SOC is not a monthly premium. It is more like a deductible. It is the amount of medical expenses you are responsible to pay for before you can get full Medi-Cal coverage for the remainder of the month. If you have no medical expenses, you pay nothing.
- More detail on how & where to pay your share of cost when you have IHSS In-Home Supportive Services Scroll down and see our references & links too.
- VIDEOs
Income Limits
To be eligible for the A&D FPL or the Blind FPL Medi-Cal programs, an applicant’s Countable Income for SSI Program cannot exceed a level set by the state that is based on the Federal Poverty Level. The countable monthly income limit for an individual adult or child is based upon the Federal Poverty Level (100% FPL), plus $230.37 Welf. & Inst. Code § 14005.40(c)(1) See Western Poverty Law Page 91 for what seems like the best and understandable explanation
Cal Matters – Problems with Income Limits – Inflations – Numbers haven’t changed in 30 years.
References & Links

- CHCF explanation SOC Share of Cost Rev December 2017
- Includes cost calculation worksheets
- CANHR Aged & Disabled Program
- CA Health Care Advocates
- Health Consumer Alliance Fact Sheet
- pascla.org/understanding-share-of-cost/
- Disability Rights CA Share of Cost – Nursing Home Resident
- Medi-Cal What it means to you Phamplet outdated?
- Covered CA Agent Certification Circa 11.2013 Page 5 et seq)
- Health Rights Hotline. Our number is 1-888-354-4474.
- 1-800-952-5253 to get a fair hearing
- Medi-Cal Contact Info
- Reddit IHSS Q & A
- Working Disabled Program – Premium may be less than Share of Cost
- Nolo – Spend Down
- Health Consumer Alliance Helping Californians get the health care they need
- McKay Law Medicaid Qualification
- CA Department of Aging Find Services
- This overview of the Medi-Cal program addresses issues relevant to older adults and persons with disabilities. At the end of this chapter is a listing of other sources of information about Medi-Cal, including information about consumer informational fliers and Medi-Cal mental health services. Bet Tsezak
- Eligibility Procedure Manual dhsc.gov
- IHSS Share of Cost
- AB 1900 to Relieve California’s Seniors, the Disabled, and Low-Income Families from the Hardship of Medi-Cal ‘Share of Cost’ Expenses
- Ways to Lower or Stop your Medi-Cal Share of Cost
- Medi-Cal Notice of Action (NOA) – Frequently Asked Questions
- Medi Cal Forms
Clarification from Hi Cap
Hello Mr. Shorr,
Mrs. Burns shared your latest email with me, and I will respond.
- First, California Health Advocates (CHA) focuses primarily on Medicare issues. We leave the topic of Medi-Cal calculations and regulations for share of cost determination to the appropriate county Medi-Cal office.
- Second, when Medicare beneficiaries request help from the local HICAP, we encounter the fact that many beneficiaries are very much connected to their Medicare Advantage Plan, and often that works against them if they have a large Medi-Cal Share of Cost (SOC) . Sometimes the only option is to return to Original Medicare during the Open Enrollment (October 15 to December 7), or other Special Enrollment Periods, and try to get a Medi gap with a premium that will help them with reducing their countable income. But then as you know, their situation would have to meet one of California’s Guarantee Issue regulations, otherwise they’d be subject to underwriting.
- Third, if a beneficiary feels that their SOC was not calculated correctly, the HICAP can refer the beneficiary to their
- Area Agency on Aging partner – Legal Services – for assistance. [Bet Tzedek – Los Angeles]
- This is the proper referral as established under the Older Americans Act.
I hope this helps with your concerns, and have to emphasize that CHA does NOT do policy or advocacy work on Medi-Cal related issues.
All the best,
Tatiana
Tatiana Fassieux
Education & Training Specialist
California Health Advocates (CHA)
Resources & Links
- Worksheets for Determining Eligibility Under the Aged & Disabled Federal Poverty Level (A&D FPL) Medi-Cal Program Disability Rights CA
- CHCF explanation SOC Share of Cost Rev December 2017
- Includes cost calculation worksheets
- Chapter 2 – DETERMINATION OF MEDI-CAL ELIGIBILITY AND SHARE OF COST
- Medically #Needy Program (CANHR Fact Sheet 8.14.2023) (My highlighted version)
- Western Poverty Law *
- CA Health Care Advocates * Read the full article from CHCF *
- AB 715 Fact Sheet *
- CHCF for 3 other examples!
- CHFC explanation of Share of Cost
- Legal Aid of San Mateo is your Share of Cost Calculated Correctly
- CA Code of Regulations Article 10 Income
-
Resources & Links
Artificial Intelligence Summary
(with our review)
While Medicare and Medicaid are primary funding sources, you can also be eligible with Medicare or through private payment if you don’t qualify for Medicaid but meet the other requirements. [1, 2, 3, 4, 5, 6, 7, 8]
- Age: You must be 55 years of age or older. [1, 2]
- Location: You must live in a geographic area served by a PACE program. [1, 3, 5]
- Nursing Home Level of Care: You must be certified by your state as needing a nursing facility level of care. This means you need a significant amount of help with daily tasks like bathing, dressing, or walking. [1, 9, 10]
- Safety: You must be able to live safely in your home or community, even with the support of PACE services. [1, 9]
- Contact your local PACE provider: Find a PACE organization that serves your area and contact them to discuss your eligibility. [9]
- We can help you. Email us [email protected]
- Assessment: The PACE interdisciplinary team will assess your physical and functional needs to determine if you qualify for a nursing home level of care. [10, 11]
- Enrollment: If you meet all the requirements, you can enroll in PACE. [9]
- With Medi Cal : If you have Medi Cal , you typically do not pay a monthly premium for long-term care services through PACE.
- With Medicare: If you have Medicare but do not qualify for Medi Cal you will pay a monthly premium for the long-term care portion of the PACE benefit.
- Private Pay: If you don’t have Medicare or Medi Cal, you may be able to pay privately for PACE services.
- my place health.com/
- myPlace Health specializes in providing value-based, comprehensive care and coverage for older adults with significant needs so they can thrive in the homes they love and in the communities they cherish.
- Our myPlace PACE (Program of All-Inclusive Care for the Elderly) model provides seamless primary care, integrated health plan coverage, personalized social engagement, and customized services – all at no cost if you are eligible for Medi-Cal or both Medicare and Medi-Cal.
- .dhcs.ca.gov/PACE
- cal pace.org/
- dhcs.ca.gov/ inclusive care for the elderly
- medicaid.gov/ /program-all-inclusive-care-elderly
- medicare.gov/PACE
- cms.gov/pace/factsheet












https://chatgpt.com/share/69c8ba13-e758-8395-8a25-3d53e5e20bba
https://apnews.com/article/medicaid-spend-down-nursing-home-care-costs-2295b93a42ecd32ea16fa9042e4c28c6
I appreciate your guidance on getting to zero share of cost, very informative! 🌟
Thank you for your help – I’ve spent years trying to figure this out and I’m glad you were able to help me.
Hi Steve,
Thank you for the nice presentation, [Loom explanation of an email] very helpful to see everything onscreen.
Best regards,
Leslie
Hi Steve,
Our zoom meeting this morning was very much appreciated.
I really benefited a lot from our discussion
Thank you very much for your assistance.
Sincerely,
Don V