
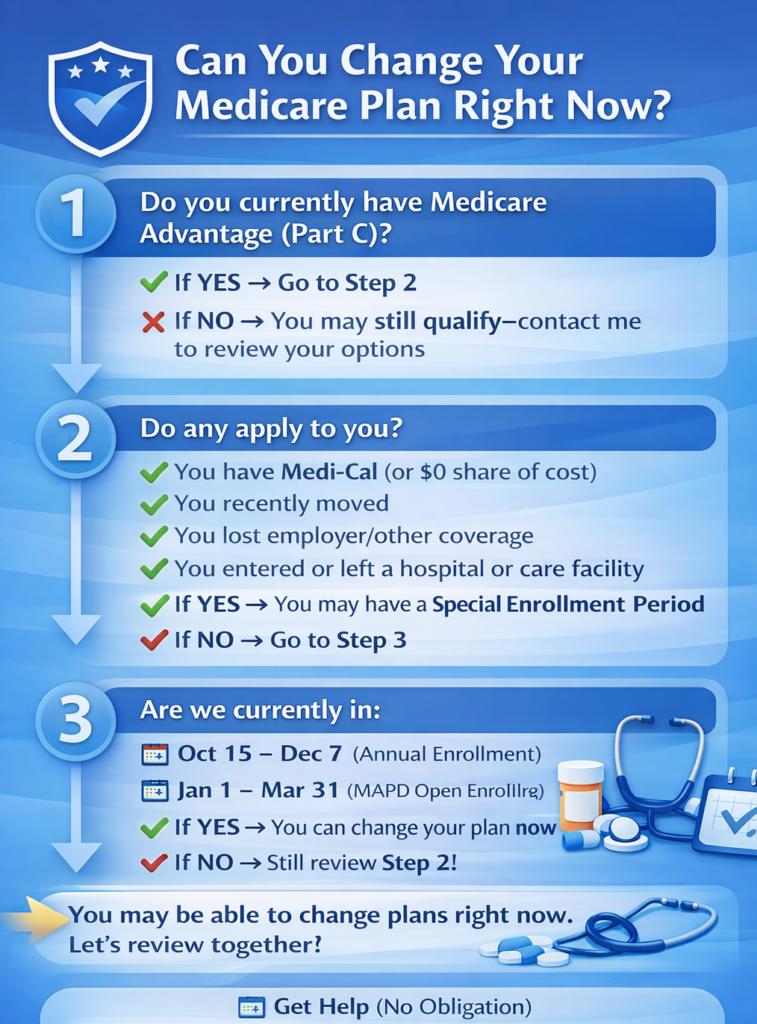
🚦 Can You Change Your Medicare Plan Right Now?
Follow this quick guide:
Step 1
Do you currently have a Medicare Advantage plan (Part C)?
👉 If YES → Go to Step 2
👉 If NO → You may still qualify—contact me to review your options
Step 2
Do any of these apply to you?
- ✔ You have Medi-Cal (or your share of cost is effectively $0)
- ✔ You recently moved
- ✔ You lost employer or other coverage
- ✔ You entered or left a hospital or care facility
👉 If YES to any → You may qualify for a Special Enrollment Period (SEP)
👉 If NO → Go to Step 3
Step 3
Are we currently in one of these timeframes?
- 📅 Oct 15 – Dec 7 (Annual Enrollment)
- 📅 Jan 1 – Mar 31 (MAPD Open Enrollment)
👉 If YES → You can change your plan now
👉 If NO → You may still qualify based on Step 2
📌 Important 2025 Update (Medi-Cal)
If you have Medi-Cal (including situations where your share of cost is effectively $0), your enrollment options changed starting in 2025.
- ✔ The old quarterly change rule was eliminated
- ✔ Some individuals may now have monthly opportunities
- ⚠️ But not all Medicare Advantage plans can be changed each time – very complex, learn more!
👉 Bottom line: You may have more flexibility—but the rules are more complex than before.
Citations DHCS.gov * Medicare.Gov * Publication 11219
🧠 What This Means for You
- ✔ You may be able to change plans right now
- ✔ You may qualify—but need to choose carefully
- ✔ You may need to wait—but exceptions often apply
👉 The only way to know for sure is to review your situation.
📞 Get Help (Fast & Easy)
Scroll down for resources, links & Citations
We do not offer every plan available in your area. Currently we represent multiple organizations which offer multiple products in your area. Please contact Medicare.gov, 1-800-MEDICARE, or your local State Health Insurance Program (SHIP) to get information on all of your options.

|
Click on link above or the chart to see the full brochure |
|
See our main page on Medicare Enrollment Periods
|
Medicare Managed Care Manual Chapter 2 Enrollment and #Disenrollment
|
Medicare MAPD & Part D Rx Enrollment Period Dates, Chart, Turn 65 ICEP, AEP, Open Enrollment Dates
#Special, Annual & Initial Enrollment Periods CHARTS
For MAPD Medicare Advantage aka Part C & Medicare + Choice & Part D Rx
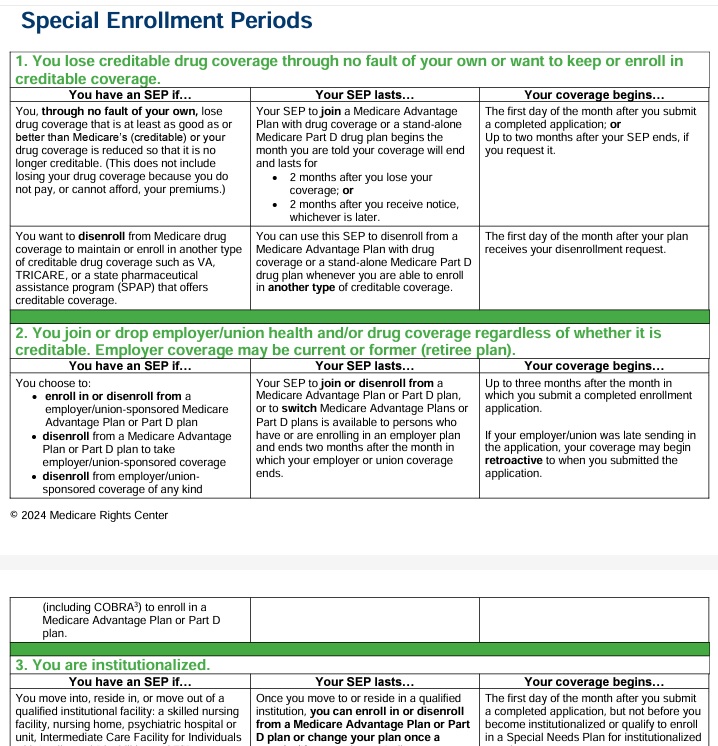
All Special Election Periods (SEP);
- Special election periods Medicare.gov constitute periods outside of the usual times when an individual may elect a plan or change his or her current plan election.
- Here's the official technical Medicare Marketing Manual or simple
- plan English, Understanding Medicare C & D enrollment periods Pub # 11219 or see
- our section on materials & guides below, there are 36 various types of SEPs, including SEPs for dual eligibles, and for individuals whose current plan terminates, who change residence and who meet “exceptional conditions” as CMS may provide, consistent with §1851(e)(4) of the Act and §422.62(b) of the MA regulations.
- When Hospitals Ditch Medicare Advantage Plans, Thousands of Members Get To Leave, Too Kff.org 4/2025
- check with us about special enrollment, like when you turn 65 or lose coverage at work.
- HI CAP CA Health Care Advocates Medicare Enrollment Periods
- Here's the official technical Medicare Marketing Manual or simple
How the Medicare Advantage Application #typically asks the "Special" Enrollment Period questions:
- I am new to Medicare.
- It's Annual Election Period aka Open Enrollment October 15th through December 7th
- I am enrolled in a Medicare Advantage plan and want to make a change during the Medicare Advantage Open Enrollment Period (MA OEP).
- I recently moved outside of the service area for my current plan or I recently moved and this plan is a new option for me. I moved on (insert date) –––––––––––.
- I recently was released from incarceration. I was released on (insert date) –––––––––––.
- I recently returned to the United States after living permanently outside of the U.S. I returned to the U.S. on (insert date) –––––––––––.
- I recently obtained lawful presences status in the United States. I got this status on (insert date) –––––––––––.
- I recently had a change in my Medicaid Medi Cal (newly got Medicaid, had a change in level of Medicaid assistance, or lost Medicaid) on (insert date) –––––––––––.
- I recently had a change in my Extra Help paying for Medicare prescription drug coverage (newly got Extra Help, had a change in the level of Extra Help, or lost Extra Help) on (insert date) –––––––––––.
- I have both Medicare and Medicaid (or my state helps pay for my Medicare premiums) or I get Extra Help paying for my Medicare prescription drug coverage, but I haven’t had a change.
- I am moving into, live in, or recently moved out of a Long-Term Care Facility (for example, a nursing home or long-term care facility). I moved/will move into/out of the facility on (insert date) –––––––––––.
- I recently left a PACE program on (insert date) –––––––––––.
- I recently involuntarily lost my creditable prescription drug coverage (coverage as good as Medicare’s). I lost my drug coverage on (insert date) –––––––––––.
- I am leaving employer or union coverage on (insert date) –––––––––––.
- I belong to a pharmacy assistance program provided by my state.
- My plan is ending its contract with Medicare, or Medicare is ending its contract with my plan.
- I was enrolled in a plan by Medicare (or my state) and I want to choose a different plan. My enrollment in that plan started on (insert date) –––––––––––.
- I was enrolled in a Special Needs Plan (SNP) but I have lost the special needs qualifications required to be in the plan. I was disenrolled from the SNP on (insert date) –––––––––––.
- I was affected by a weather-related emergency or major disaster (as declared by the Federal Emergency Management Agency (FEMA). One of the other statements here applied to me, but I was unable to make my enrollment because of the natural disaster
More SEP’s Special Enrollment Periods
When can you change MAPD plans if you have Medi Cal?
Google AI
- Integrated Care SEP (Monthly): Full-benefit dually eligible individuals can enroll in or switch between qualifying integrated D-SNPs once per month. These are plans specifically designed to align Medicare and Medicaid coverage under one insurer.
- Monthly SEP for Standalone Plans: This SEP allows switching between standalone Prescription Drug Plans (PDP) or disenrolling from a Medicare Advantage plan to return to Original Medicare once per month.
- Restriction on Regular MAPD Plans: This monthly SEP cannot be used to switch from one regular Medicare Advantage plan to another regular Medicare Advantage plan. To switch between non-integrated plans, beneficiaries must wait for standard periods like the Annual Enrollment Period (Oct 15 – Dec 7) or the Medicare Advantage Open Enrollment Period (Jan 1 – March 31). [2, 3, 4, 5, 6, 7, 8]
| Action [2, 3, 4, 5, 8] | Frequency | Plan Requirement |
| Switch to Integrated D-SNP | Once per month | Must be a FIDE SNP, HIDE SNP, or Aligned AIP |
| Switch Standalone Drug Plans | Once per month | Standalone PDP only |
| Return to Original Medicare | Once per month | Disenroll from MA/MAPD |
| Switch Regular MAPD Plans | Annual/Standard windows | Standard enrollment periods apply |
- Partial-Benefit Duals: Those who only receive “Extra Help” (LIS) or have partial Medicaid benefits do not qualify for the integrated care monthly SEP. They generally must wait for standard open enrollment periods to change Medicare Advantage plans.
- Effective Dates: Any plan changes made using these monthly SEPs take effect on the first day of the following month.
- Medi-Cal Medical Plans: Separate from Medicare, if you are unhappy with your Medi-Cal managed care medical plan, you can generally choose another available Medi-Cal plan by contacting Health Care Options. [3, 5, 7, 8, 9, 10, 11]
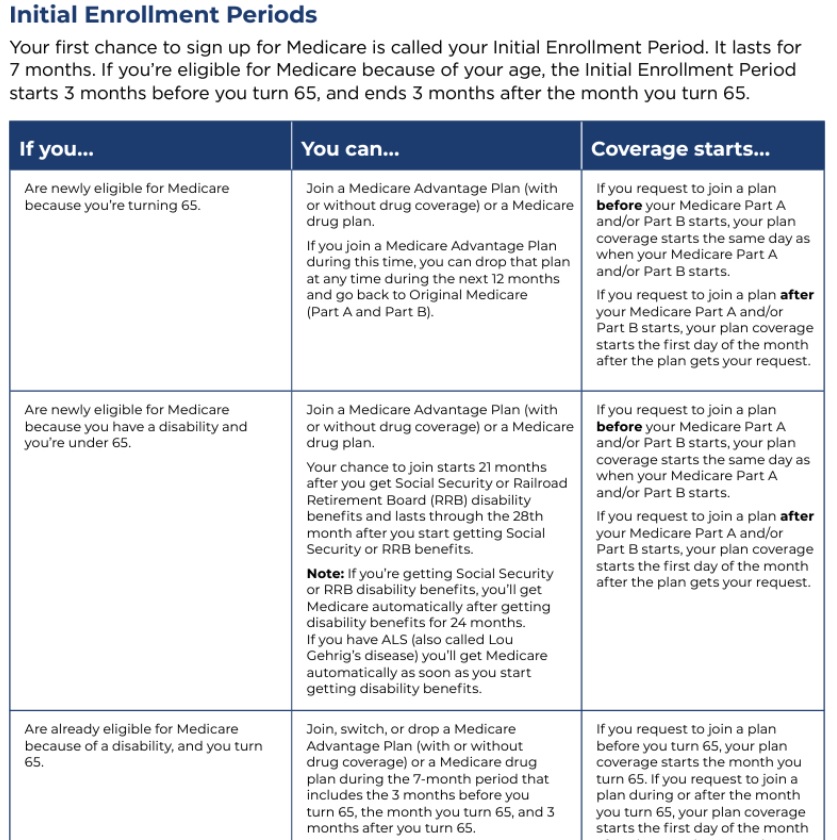
When you Turn 65
When you #turn65
The Initial Coverage Election Period (ICEP)
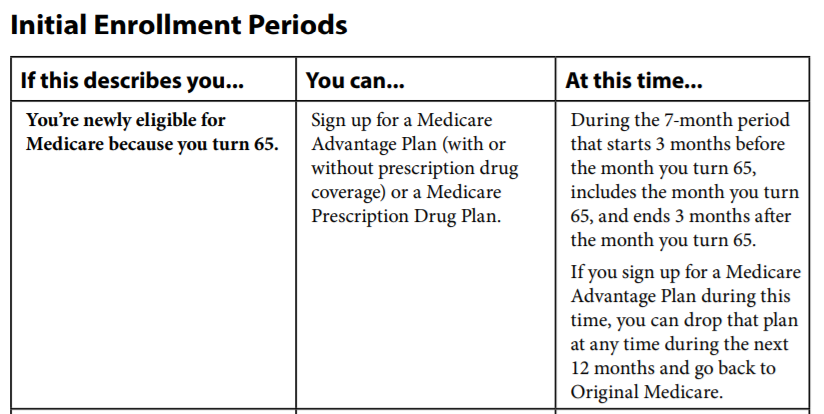
- The ICEP (Initial Enrollment Period – turn 65 – SSDI enrollment) is the period during which an individual newly eligible for Medicare Advantage may make an initial enrollment request to enroll in an MA plan. This period begins three months immediately before the individual’s first entitlement (Turning 65) to both Medicare Part A and Part B and ends on the later of:
- 1. The last day of the month preceding entitlement to both Part A and Part B, or;
- 2. The last day of the individual’s Part B initial enrollment period.
- The initial enrollment period for Part B is the seven (7) month period that begins 3 months before the month an individual meets the eligibility requirements for Part B, and ends 3 months after the month of eligibility. See 42 CFR 407.14 for additional information.
- Once an ICEP enrollment request is made and enrollment takes effect, the ICEP election has been used. Section 30.2 * Understanding Medicare Enrollment Periods # 11219 *
- Yes, I know this is all very complicated! Email us for assistance.
- Application for Medicare Part A and Part B Special Enrollment Period (Exceptional Circumstances) Cms.Gov pdf 7/2025
Jump to section on:
- Medicare Advantage Open Enrollment Period ( MA OEP)
- Part D IEP Initial Election Period
- Annual Election Period (AEP) §30.1
- ACA – Obamacare – under 65
- Turn 65 Initial Coverage Election Period (ICEP)
- Medi Gap – Supplemental
- Special, Annual & Initial Enrollment Periods
- Medicare Part B Dr. Visits & Outpatient
The Medicare Advantage Open Enrollment Period
( #MAOEP)
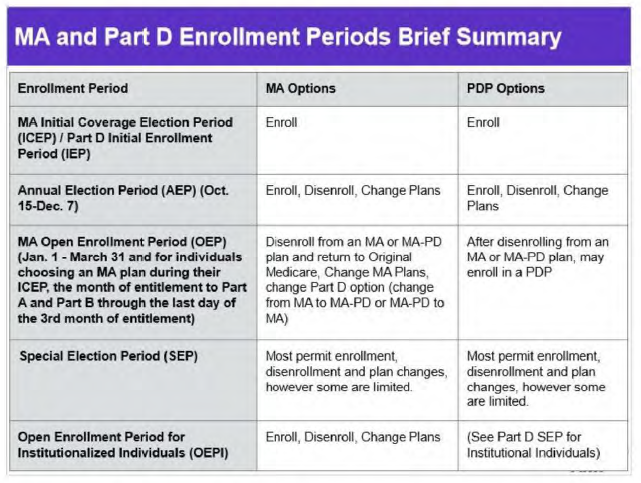
- During the MA OEP Open Enrollment Period, MA plan enrollees may enroll in another MA [PD] plan or disenroll from their MA [PD Prescription] plan and return to Original Medicare. Individuals may make only one election during the MA OEP.
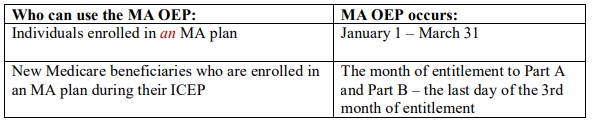
- This chart outlines who can use the MA OEP and when:

- Individuals enrolled in an MA [PD] plan may add or drop Part D coverage during the MA OEP. Individuals enrolled in either MA-PD or MA-only plans can switch to:
- • MA-PD
• MA-only
• Original Medicare (with or without a stand-alone Part D plan)
And see if they qualify for a Medi Gap plan - Check the ANOC Annual Notice of Change from your Medicare Advantage plan - if any benefits are lower... that may get you guaranteed issue into Medi Gap!!!
- The effective date for an MA OEP election is the first of the month following receipt of the enrollment request.
- NOTE: The MA OEP does not provide an opportunity for an individual enrolled in Original Medicare to join a MA plan. It also does not allow for Part D changes for individuals enrolled in Original Medicare, including those enrolled in stand-alone Part D plans. The MA OEP is not available for those enrolled in Medicare Savings Accounts or other Medicare health plan types (such as cost plans or PACE). Medicare Managed Care Manual Chapter 2 * Section 30 - Election Periods * CA Health Advocates.org * 42 CFR §§ 422.62 & 422.68 * Medicare & You *
- You have the opportunity to make one change to your health coverage during the annual Medicare Advantage Open Enrollment Period.
- HI CAP CA Health Care Advocates Medicare Enrollment Periods
- FAQ's
- What type of plan can you switch to during the annual Medicare Advantage Open Enrollment Period?
- During this time, you can:
- Switch to another Medicare Advantage plan. (You choose a plan that covers prescription drugs or one that does not cover prescription drugs.)
- Disenroll from an MAPD plan and obtain coverage through Original Medicare.
- You can apply for Medi Gap, but it may not be guaranteed issue and require underwriting. If that's your plan, get approved for Medi Gap FIRST!!!
- If you choose to switch to Original Medicare during this period, you have until March 31 to join a separate Medicare prescription drug plan to add drug coverage. We are not interested in writing people though who wait till the last minute. If that's your plan please find another agent or go direct to Medicare.Gov Things get lost...
- When will your membership end?
- Your membership will end on the first day of the month after you enroll in a different Medicare Advantage plan or we get your request to switch to Original Medicare. If you also choose to enroll in a Medicare prescription drug plan, your membership in the drug plan will begin the first day of the month after the drug plan gets your enrollment request. Evidence of Coverage §2.2 page 240 * Medicare Managed Care Manual Chapter 2 * 42 CFR 422.62(a)(3) * insuremekevin.com/new-medicare-advantage-open-enrollment-period-for-2019/
- Resources & Links
- VIDEO by Nick Williams on MAPD NEW Open Enrollment Period
- CA Health Advocates.org
- Medicare & You
- Ritter.com Rules for agents on what you can and can't do
Video is for Agents – Sales Training
The Annual Election Period (#AEP) aka Open Enrollment §30.1
- AEP – Annual Enrollment starts October 1st is when you can get the next years information, rates, benefits, etc. Then on October 15 through December 7 every year you can enroll or change your plan. Medicare Advantage and Part D Rx eligible individuals may enroll in or disenroll from a Medicare Advantage or Part D Plan plan. Publication 11219 *
- We offer:
- The last enrollment request made, determined by the application date, will be the enrollment request that takes effect. CMS.gov *

Federal Emergency Management Agency (#FEMA)
- Location/Impact: You lived in a declared disaster area, or your helper lived there, during the incident period.
- Eligibility: You were eligible for a standard enrollment period (like Annual Enrollment) when the disaster struck.
- Missed Election: You didn't make a plan choice during that time because of the disaster/emergency. [1, 2, 3, 4]
- Government Declaration: A federal, state, or local government entity must declare the disaster/emergency (e.g., FEMA).
- Duration: The SEP typically lasts for the emergency period plus an additional two months after the end of the incident period.
- Use on Applications: Use "SEP DST" as the election code for this special period when applying. [2, 3, 4, 5]
- Special Election Issues for Individuals Affected by Declared Emergencies and Disasters
- Special Enrollment Periods for complex issues Medicare.Gov
- fema.gov/disaster
- Special Enrollment Period (SEP) for Individuals Affected by a FEMA-Declared Weather-Related Emergency or Other Major isaster: Applicable for COVID-19
- Ritter GA
- HI 00805.383 CMS.gov
- FEMA Declared Disasters Search tool fema.gov
Trying to prove Contract Violations???
30.4.2 – SEPs for Contract Violation
In the event an individual is able to demonstrate to CMS that the MA organization offering the MA plan of which he/she is a member substantially violated a material provision of its contract under MA in relation to the individual, or the MA organization (or its agent) materially misrepresented the plan when marketing the plan, the individual may disenroll from the MA plan and elect Original Medicare or another MA plan.
The SEP will begin once CMS determines that a violation has occurred. Its length will depend on whether the individual immediately elects a new MA plan upon disenrollment from the original MA plan or whether the individual initially elects Original Medicare before choosing a new MA plan. Medicare Managed Care Manual Chapter 2
Our webpage on
The Open Enrollment Period for Institutionalized Individuals (OEPI)
- The OEPI is continuous for eligible individuals. For purposes of enrollment under the OEPI election period, an institutionalized individual is defined as an individual who moves into, resides in, or moves out of an institution, as defined in §10. The OEPI ends two months after the month the individual moves out of the institution. Medicare Managed Care Manual § 30.3 *
#Initial Enrollment Period for Part D Rx
(IEP for Part D) §30.2.1
- In general, an individual is eligible to enroll in a Part D plan when he or she is entitled to Part A OR is enrolled in Part B, AND permanently resides in the service area of a Part D plan.
- During the IEP for Part D, individuals may make one Part D enrollment choice, including enrollment in an MA-PD plan.
- Generally, individuals will have an IEP for Part D that is the same period as the Initial enrollment Period for Medicare Part B.
Additional Resources & Links
Reference Materials
- Medicare and You #10050 for an introduction or
- Medicare Rights – 16 page pdf on Special Enrollment Periods for Advantage and Part D Plans
- Medicare Managed Care Manual Chapter 2 * Section 30 – Election Periods
- CA Health Advocates.org
- Medi-Gap Dates & Guaranteed Enrollment on this website.









https://cahealthadvocates.org/surprised-to-find-your-doctor-not-in-your-ma-plan-you-may-qualify-for-a-new-special-enrollment-period/
https://cahealthadvocates.org/medicare-advantage/enrollment-disenrollment-in-medicare-advantage-plans/
https://cahealthadvocates.org/surprised-to-find-your-doctor-not-in-your-ma-plan-you-may-qualify-for-a-new-special-enrollment-period