Medicare Coverage for Diabetes under Parts A Hospital and B Doctor Visits
Medicare Coverage for Diabetes # 11022
VIDEO's
- Diabetes Official Medicare VIDEO
- Max Insulin Co Pay $35
- Sugary Drinks - No Good VIDEO
- HBO Weight of the Nation VIDEO
- Fed UP – Official Trailer VIDEO
- Beat Diabetes – VIDEO You Tube - A trip to the grocery store
- Trump – Lower Cost of Insulin 5.26.2020 VIDEO
- How to use Medicare Part D Rx Plan Finder VIDEO
- Our main webpage on diabetes
- Rated – Surcharged Policies Pre Existing Conditions
- Stelo - Watch and Learn

Blue Cross Anthem Authorized Broker
- Instant quotes & #Enrollment for Individual & Family
- Employer Small Group Health Proposals - Quotes
- We’re here to help you with any enrollment, selection and service questions you might have. Anthem pays us to help you at no extra charge! Check out the brochures below and on either side.
What Medicare Covers for Diabetes
Diabetes screenings
Medicare covers these screenings if your doctor determines you’re at risk for diabetes or diagnosed with prediabetes. You may be eligible for up to 2 diabetes screenings each year. You pay nothing for the test if your doctor or other qualified health care provider accepts assignment.
Medicare Diabetes Prevention Program
Prediabetes is a serious health condition where blood sugar levels are higher than normal, but not high enough yet to be diagnosed as having type 2 diabetes. Fortunately, type 2 diabetes can sometimes be delayed or prevented with health behavior changes. If you have prediabetes, losing even a small amount of weight if you’re overweight and getting regular exercise can lower your risk for developing type 2 diabetes.
If you have Medicare Part B, have prediabetes, and meet other criteria, Medicare covers a proven health behavior change program to help you prevent diabetes. The program begins with at least 16 core sessions offered in a group setting over a 6-month period. After the core sessions, you may be eligible for additional monthly sessions will help you maintain healthy habits.
The diabetes prevention program sessions will include:
• Training to make realistic, lasting lifestyle changes
• Tips on how to get more exercise
• Strategies for controlling your weight
• A lifestyle coach, specially trained to help keep you motivated
• Support from people with similar goals and challenges
If you think you’re at risk, ask your doctor to be tested for prediabetes to find out if you have the condition. If you qualify for the program, you can join a program at no out-of-pocket cost without a referral from your doctor. If you’re in a Medicare Advantage Plan, contact your plan for more information.
- medicare.gov/medicare-diabetes-prevention-program
- cdc.gov/diabetes/prevention
- Vision – Keep your eyes healthy Blue Shield website
Diabetes self-management training
Medicare covers diabetes outpatient self-management training to teach you to cope with and manage your diabetes. The program may include tips for eating healthy, being active, monitoring blood sugar, taking medication, and reducing risks. You must have diabetes and a written order from your doctor or other qualified health care provider who’s treating your diabetes. You pay 20% of the Medicare-approved amount, and the Part B deductible applies.
Diabetes supplies
Medicare covers blood sugar testing monitors, blood sugar test strips, lancet devices and lancets, blood sugar control solutions, and therapeutic shoes (in some cases). Medicare only covers insulin if it’s medically necessary and you use an external insulin pump to administer the insulin. You pay 20% of the Medicare-approved amount, and the Part B deductible applies.
Note: Medicare prescription drug coverage (Part D) may cover insulin, certain medical supplies used to inject insulin (like syringes), and some oral diabetes drugs. Check with your plan for more information. Medicare & You #10050
By submitting the information below , you are agreeing to be contacted by Steve Shorr a Licensed Sales Agent by email, texting or Zoom to discuss Medicare or other Insurance Plans as relevant to your inquiry. This is a solicitation for Insurance
Ways to #Manage Type 2 Diabetes
- How healthy eating leads to reduced spending on prescription drugs, emergency room visits and hospitalizations
- Our webpage on nutrition & weight control
- cdc.gov/diabetes
- healthy.kaiserpermanente.org//diabetes
- Step-by-Step Guide to Medicare Medical Nutrition Therapy (MNT) Reimbursement
- niddk.nih.gov/preventing-type-2-diabetes
- my diabetes.diet
- so yummy.com/away-foods-stay
- Foods to stay away from
- 14 hour fast works wonders latimes.com/time-restricted-eating-intermittent-fasting-metabolic-syndrome
- Blue Shield Care Management Program
- Get your life back–and leave diabetes behind
Virta can help you learn how to improve blood sugar and lose weight, so you can get back to what you love.
Virta is available at no additional cost to eligible Blue Shield of California members. Blue Shield *
- Get your life back–and leave diabetes behind
- What happens when you drink a Soda
- Food and diet can help a lot time.com/food-best-medicine/
- i waste so much money.com/foods-that-can-help-with-diabetes/
- does-medicare-cover-nutrition-counseling
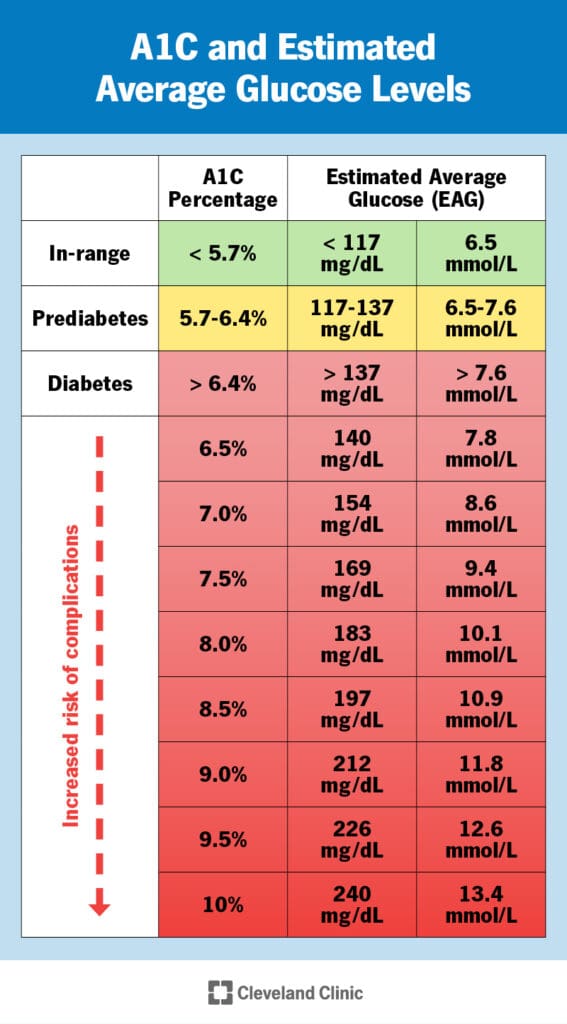
- What are normal blood glucose levels Singlecare.com
- Dental care reduces likelihood of hospitalization for people with diabetes or coronary artery disease Medical Press 5.6.2022
- Blood sugar self-testing equipment & supplies
- Insulin pumps
- Our webpage on Medicare Advantage SNP Special needs plans
- Clinical Guidelines – Medical Necessity
- Therapeutic shoes or inserts Medicare.Gov
- Medicare Part D Rx Diabetes Coverage 11022
- Insulin
- Anti-diabetic drugs
- Diabetes supplies
- Medicare-Covered Diabetes Services
- screenings
- self-management training
- Medical nutrition therapy services
- Foot exams & treatment
- Hemoglobin A1c tests
- Glaucoma tests
- Flu and pneumococcal shots (vaccinations)
- “Welcome to Medicare” preventive visit
- Yearly “Wellness” visit
- Supplies & services that aren’t covered by Medicare
- Tips to help control diabetes
- Diabetes & the Affordable Care Act ncbi.nlm.nih.gov
- Coverage for Diabetes At-a-Glance
- Part B-Covered Diabetes Supplies
- Formulary issues?
- Medicare Coverage for Diabetes Publication # 11022
- Web MD on Diabetes
- Sharp HealthCare offers a diabetes education program
- Intermittent Fasting Web MD
- Sleep Apnea Web MD
- Control Diabetes during workout
- Acid reflux drugs may increase risk of type 2 diabetes
- medicare.gov/diabetes-prevention-program#/
- How is diabetic nerve pain treated
Blue Shield of California Authorized Agent - Broker
![]()
How disabled from diabetes must you be to get disability –
SSI, SSDI or California SDI?
- disability-benefits-help.org/diabetes-and-social-security-disability
- nolo.com/can-you-get-disability-for-diabetes
- disability secrets.com/social-security-disability-diabetes
- nick ortiz law.com/disability-for-diabetes-type-i-or-ii-diabetic-neuropathy
- oc disability attorneys.com/disability-benefits-for-diabetes-mellitus
- SSA.Gov Evaluating Diabetes Mellitus
- web md.com/diabetes-should-apply-disability
- medical news today.com/is-type-2-diabetes-a-disability
See our webpages on:
Prescription Drug 2025 #RxGuide
PDF # 11109
*****************
No more Coverage Gap - Donut Hole $2,100 Cap

******************
- Medicare Part D Rx premiums can be found on Medicare . Gov See instructions on how to shop premiums.
- Scope of appointment - permission to discuss Rx and MAPD Plans
- Our Webpage Premiums for those with High Income Parts D Rx & B Doctor Visits
- Medicare Rules for High Income People Medicare Costs # 11579
- Our #High Income Surcharge Video Explanation
- Kaiser Foundation Introduction - Overview
- Fact Sheet Medicare Part D CA Health Care Advocates Hi Cap
-
. Prescription Drugs Hi Cap
- Medicare Part D: An Overview – 10-31-23
- Prescription Drug Resources – 11-07-22
- When Your Part D Prescription is Denied– 11-22-22
- Shop & Compare Tools Part D Rx
- Get Instant Quotes, Information & Enroll online
- See our web page on Part D Shop & Compare for more information & FAQ's
- MANDATED wording!: ‘‘We do not offer every plan available in your area. Any information we provide is limited to those plans we do offer in your area. Please contact Medicare.gov or 1–800–MEDICARE to get information on all of your options.’’ § 422.2267(e)(41).
- We disagree with the above wording, as we can use the same tools on Medicare.gov as they do!
Maximum Co Pay for #Insulin $35?
Part D plans (shop & compare here or email us) can offer insulin at a monthly copayment of no more than $35.
The new insulin model directly addresses this disincentive by doing two things:
1) allowing manufacturers to continue paying their full coverage gap discount for their products, even when a plan offers lower cost-sharing; and
2) requiring participating Part D sponsors’ plans, in part through applying manufacturer rebates, to lowering cost-sharing to no more than $35 for a month’s supply for a broad set of insulins.
CMS is enabling and encouraging Part D plans to offer fixed, predictable copays for beneficiaries rather than leaving seniors paying 25 percent of the drug’s cost in the coverage gap. Both Big Pharma - manufacturers and Part D Insurance Companies responded to this market-based solution in force and seniors that use insulin will reap the benefits. KFF.org *
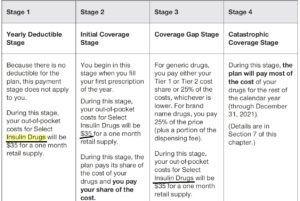
Here's how it's explained in a "Sample" EOC Evidence of Coverage. Click on image to enlarge
Resources & Links
- Wait, Is Insulin Cheaper Now? KFF 2.28.2024
- Why won’t Medicare deliver food to sick seniors, if it could get them healthy?
- Many diabetics ration or don't take their full doses as they don't have the $$$ to pay for their insulin. LA Times 10.7.2021 *
- Los Angeles Times - Trumps claim insulin is cheap, is not accurate
- cal matters.org/insulin-costs-california
- npr.org/house-passes-bill-to-cap-insulin-prices
- H.R.6833 - Affordable Insulin Now Act
- Senators Unveil Bill That Would Cap Insulin Costs For Many
- 1.2 million Americans spent more than 40% of income on insulin: study
- Insulin is an extreme financial burden for over 14% of Americans who use it
- California To Manufacture Its Own ‘Low Cost’ Insulin
- Covered CA and direct - under 65 Rx Prescription Formularies
- Many insulin users face "catastrophic spending"
- Diabetes advocates frustrated after insulin cost cap is dropped from drug pricing bill
- $300 more for the same insulin: The Medicare rule that makes pump users pay more
- The Inflation Reduction Act caps costs for Medicare patients on insulin. Where the push for broader relief stands
- Our webpage on Inflation Reduction Act
- More than 1.3M Americans ration life-saving insulin due to cost. That's 'very worrisome' to doctors.
- Medicare Plan Finder Likely Won’t Note New $35 Cap on Out-of-Pocket Insulin Costs
- Type 2 diabetes patients struggle with expenses, stress It was also revealed that 32% of people living with Type 2 diabetes don't trust the U.S. healthcare system to keep them healthy.
- New Diabetes Drug To Cost $13,850 Per Vial, More Than Some Estimates
Get More Details
- Medi Gap – Supplement Plans – non conical
- Anthem Blue Cross
- Blue Shield – Medi-Gap – Any Medicare Provider
- Guaranteed Acceptance – Medi-Gap – Supplemental Plans
- Health Net Medi Gap
- UnitedHealthcare Medi Gap
- Medicare Advantage Plans – Part C
- Anthem MediBlue Plus & SNP
- Blue Shield 65 Plus – Inspire HMO 2024
- Original Medicare & Medi-Gap – Supplement vs Medicare Advantage MAPD
- Scan
- SNP Special Needs Plans Medicare Advantage
- UnitedHealthcare
-
Brother – Sister – Sibling Side Pages Subpages
- Email us [email protected]
- Term Life Insurance – Diabetic Questionnaire New Generation