Anthem Blue Cross

Individual & Family Health Insurance Plans
- We are Blue Cross – Anthem ♦ Authorized Agents Broker # GFKGQSJSRZ and are happy to help you get covered in CA at no extra charge to you. Blue Cross pays us to help you find their best plan that fits your needs. Here are a few of the many benefits that an agent/broker can provide to the public.
- The BEST way to get the most current specific brochures and rates for each plan is click here.
- Under ACA/ObamaCare there are no pre x and enrollment is guaranteed during Open Enrollment and when you qualify for a Special Enrollment
- Then we can do a Zoom meeting to review and complete the application

- Instant quotes & #Enrollment for Individual & Family
- Get the latest and most updated information.
- Medicare information contact us [email protected]
- Employer Small Group Health Proposals - Quotes
- We’re here to help you with any enrollment, selection and service questions you might have. Anthem pays us to help you at no extra charge! Check out the brochures below and on either side.
2024 ONLINE Brochure - we are waiting for pdf
Off Exchange - Direct Benefit Chart 2024
- 2024 - All Plans - 6 languages
- Product Guide Direct - Not Covered CA
- Steve's VIDEO Introduction to the brochure
- Anthem VIDEO on subsidies and options
- Silver HMO EOC Evidence of Coverage-Plain English VERY informative!
- Anthem.com/ca/pharmacy – Formulary information
- Covered CA - Online Application through Quotit
- Medical Policies & Clinical UM Guidelines
- Paper Application, but ONLINE is better
- Email us [email protected]
All our plans are Guaranteed Issue with No Pre X Clause
Quote & Subsidy #Calculation
There is No charge for our complementary services
Watch our 10 minute VIDEO
that explains everything about getting a quote
- Our Quote Engine Takes all the complexity out of using pencil and paper to figure out the premiums per the Obamacare/ACA rules under CFR §1.36B-3 *
- Get more detail on the Individual & Family Carriers available in CA
Member Portal
Blue Cross #MemberPortal

Manage claims, your health, preventative benefits, find doctors, plan details, benefits, refill rx, health assessment and compare costs
- Login In or Register
- Bank Draft Form
- FAQ’s Go Paperless
- Q: Do I have to go paperless?
- A. Not at all. The choice to go paperless or stick with paper claim summaries is up to the subscriber. But going paperless is a great option.Here’s a 2 page pdf on how to read Blue Cross’s EOB
More information on Claims Payment Policies & Practices
Here’s a Blue Cross subsidiary’s answer!
How do I get a paper EOB?
Answer: You may contact Member Services at the telephone number listed on your ID card to obtain a paper copy of an EOB. Carefirst
If you appoint us as your broker, no extra charge, we can do this for you.
- Claim Forms
Contact #'s
- Check the back of your ID card
- Website Technical Support 1-866-755-2680
- 800-928-6201-Part D Customer Service Phone number
- 800 333 3883-Med Supp Customer Service phone number
- Medicare Advantage Member Services
- (1) HMO Customer Service 888-230-7338
- (2) HMO DSNP Customer Service 844-469-6831
- (3) PPO Customer Service 877-811-3107
- (4) ESRD PPO SNP Customer Service 844-648-9540
Sydney App for iPhone and Android
-
Find care and check costs: It’s easy to search for doctors, dentists, hospitals, labs and other providers in your plan. You can search by name, location and type of care. You can even filter by gender or languages spoken, then check costs before you go. This helps you find what’s best for you.
-
View claims: With one click, you can check claims. That means you can spend more time focused on your health and less on managing your health benefits.
-
View and use digital ID cards: You can always have your most current ID card handy. And you can use it just like a paper one when you visit the doctor, dentist, pay for care and more.
-
See all benefits: Sydney shows you essential information at a glance, whether that’s an overview of your plan, health reminders or suggestions for wellness programs. You also can find your deductible, copay and share of costs.
-
Use the interactive chat feature and get answers quickly: Simply type your questions in the app and get answers quickly. Plus, Sydney can suggest resources to help you understand your benefits, improve your health and save money.
-
Check My Family Health Records (myFHR): myFHR gives you easy access to your health data, including health history and electronic medical records, all in one place. Availability is based on your plan.
Investor & Financial Strength
- Annual Reports
- Wellpoint – Ethical Standards 2006
- Wikipedia on BS/BC
- WellPoint, Inc. Code of Conduct
- Investor Information & Financial Strength
Networks & Provider Finder
Provider Lists – Definitions
HMO, EPO
WHAT SHOULD I KNOW ABOUT MY NETWORK?
Exclusive provider organization (EPO):
With our EPO plans, you’ll be able to see any in network doctor, no PCP required. Email dated 1.7.2022 9:32 AM * It’s a good idea to have a primary care doctor to coordinate your care, so we’ll pick one close to your home and let you know your assignment in the beginning of the year. You don’t need to see this doctor for services or referrals, and you can change your assigned primary care doctor at any time.
EPO plans don’t offer out of network benefits, except for emergency and urgent care, ambulance services or when a service is pre approved. If you see a doctor not in your plan for any other reason, you’ll have to pay 100% out of pocket.
Health maintenance organization (HMO):
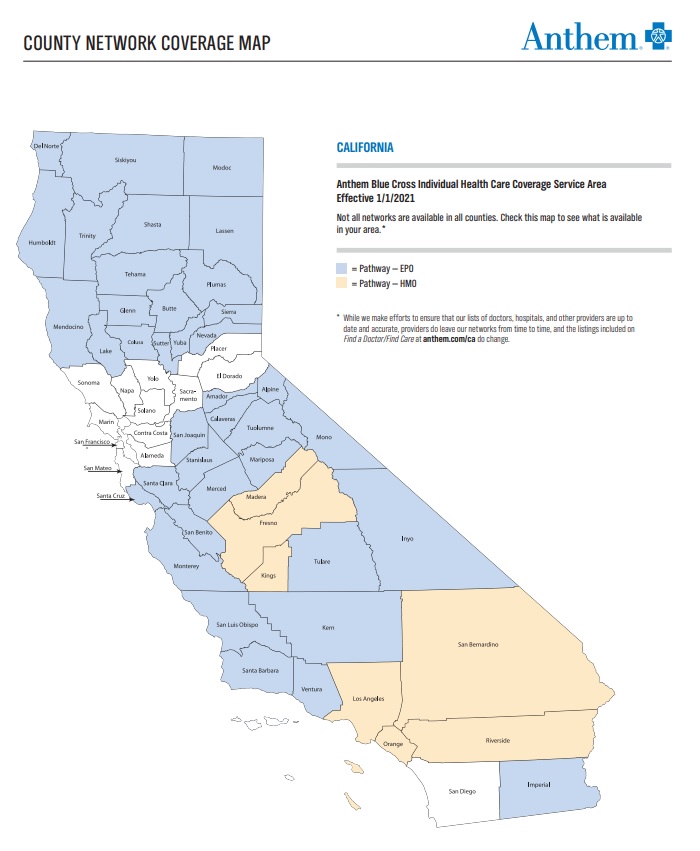
With an HMO, you have to choose a primary care doctor to manage your care needs — including getting referrals to see other network doctors. HMOs don’t offer out of network benefits, except for emergency and urgent care or when a service is pre approved. If you see a doctor not in your plan for any other reason, you’ll have to pay 100% out of pocket HMO plans are available in Fresno, Kings, Los Angeles, Madera, Riverside and San Bernardino counties Brochure * 2021 Brochure *
Basically, a PPO allows one to go out of network, but the reimbursement will be less. See your summary of benefits or EOC Evidence of Coverage for Blue Shield PPO Silver 70
Participating (Participating Provider)
A provider who participates in this plan’s network and contracts with Blue Shield to accept Blue Shield’s payment, plus any applicable Member Cost Share, as payment in full for Covered Services. Also referred to as an in-network provider.
Preferred Provider Organization (PPO)
A type of health benefit plan designed to give enrollees incentives to use health care providers designated as “preferred providers”, but that also give substantial coverage for services received from other health care providers.
PPO plans can also be distinguished from HMO plans by the ability of PPO members to see any specialty physician without referral from a PCP, although some HMOs with a POS feature may allow this as well. See also HMO See our HMO, EPO & PPO page
#Find a Anthem Blue Cross
Doctor, Physician, Dentist Hospital and other Providers
- Network Map Individual & Family Plans
- What plans do major providers accept?
- Cedar’s Sinai,
- UCLA
- Health Care Partners – Optum,
- THIPA Torrance Memorial IPA
-
Blue Cross Removes UC Hospitals From EPO Health Plans
UC Davis Medical Center, UC San Francisco Medical Center and Children’s Hospital, along with Benioff Children’s Hospital in Oakland are no longer part of their Pathway EPO network as January 1, 2022 Learn More - Insure Me Kevin.com
- Clinical utilization management (UM) guidelines focus on selection criteria, length of stay, and location for generally accepted technologies or services.
- Anthem Blue Cross Provider List Definitions Individual Plans
- Enroll with Blue Cross Anthem
- VIDEOS
- What to do when you receive a doctor bill VIDEO
- VIDEO When you're looking for health insurance in California, consider the quality of care provided by Anthem Blue Cross. The Anthem team knows the needs of growing families and offers an array of plans that offer affordable coverage for members of all ages.
- VIDEO What do do when you get a doctor's bill
- Live Health ONLINE - Tele Med with therapist VIDEO
- SYDNEY Overview VIDEO
- In & Out of Network - What's a network? HN Video
- Steve helps you find PCP VIDEO
Dental & Vison
Anthem Blue Cross California Individual & Family
#Dental Net 3000 d, Prime, Blue Plans
Dental Plans cover things like Root Canals, Dentures, Braces, routine cleaning.
Blue Cross Anthem Dental & Vision Brochure 2025
-
- 2025 Benefit Charts
- enroll ONLINE
- Blue View Vision * Premiums *
- Dental Premiums
- Term Life *
- Participating Dentist Finder
- Email us ([email protected]) for Blue Cross details.

Oral Health for #Seniors
Justice in Aging - Advocates Guide Updated 2025
- Denti-Cal under Medi Cal
- National Institute for Dental Research - Caregiver information
- Health.Gov tips for older adults
- nia.nih.gov/taking-care-your-teeth-and-mouth
- Dental Care - Medicare
#Importance of Dental Coverage
Dental & General Health
Insurance 101?
We suggest that you check out Life Insurance, Disability, Long Term Care and Retirement as these risks may cause much more financial devastating to your budget than dental bills.
Picture of Oral Health
- Dental For #Everyone, Instant Quotes - Online Enrollment
-

Delta Dental - Get Quotes & Enroll
- Dental care reduces likelihood of hospitalization for people with diabetes or coronary artery disease Medical Press 5.6.2022
- The 2022 State of America’s Oral Health and Wellness Report Commissioned by Delta Dental Plans Association
- What drives buyers of individual Delta Dental plans?
- 77 Million Adults Do Not Have Dental Insurance
- CDA-sponsored bills seek more protections, increased oversight of dental insurance Bills would prohibit plans from imposing arbitrary waiting periods, denying coverage for preexisting conditions; require rate review and ERISA notice Learn More >> CDA * CA Legislature * California Benefits Review Program *
Steve on buying, shopping and best use of premium dollars
Dental Insurance VIDEO
MORE VIDEOS
- What dental Insurance... should I buy???
- VIDEO the dentist attempts to give you some guidance about things to consider before buying a dental insurance plan, finance plans available, negotiating with your dentist
- Sacramento Truck driver sudden dealth from tooth infection Sacramento Bee 1.31.2017
- Health Savings Accounts?
- Video - how bad sugary drinks are for you
Our other pages on
Dental Coverage
We don't put a lot of effort into selling dental coverage. Generally it's a wash on paying premiums vs getting back claims payments. Unless it's employer group. Then the premiums are tax deductible under IRS Section 106.
Here's more information on how we feel about dental. Here's our page on implants, where we get lots of inquires, but few sales. Most people only seem to want dental coverage, after they've been told they need a lot of dental work. Not profitable for Insurance Companies. See our other pages for details & explanations. See our page on Medical Loss Ratio. Insurance Companies need to take in $1 to pay 80c in claims.
Medicare Plans
- Anthem Blue Cross
- Blue Shield – Medi-Gap – Any Medicare Provider
- Health Net Medi Gap
- UHC AARP Medi Gap
- Scan
Individual & Family Plans
Dental For Everyone,
has an excellent website with full brochures, Instant online quoting and enrollment
One of our colleagues on how Dental for Everyone Works..
Employer Group Plans
- Medi-Cal
Medi Cal
Grandfathered Plans & Historical
FAQ’s
In California Blue Cross and Blue Shield are two totally different and separate companies. See our webpages…
What is a (Blue Cross or Shield) #Multi State Plan under the Affordable Care Act?
The Multi-State Plan (MSP) Program, established under the Affordable Care Act, directs OPM [Federal Office of Personnel Management*] to contract with private health insurers in each State to offer high-quality, affordable health insurance options called Multi-State Plans OPM.Gov FAQ’s
Multi-State Plans are overseen by the U.S. Office of Personnel Management (OPM) and are similar to the other Qualified Health Plan products offered on the exchanges. Generally, all of the same requirements that apply to other products also apply to these Multi-State Plan products. The name “Multi-State Plan” does NOT mean that consumers have health plan coverage for non-urgent care in multiple states. Excerpt from Agent Guide
OPM’s claim to fame appears to be that they have 50 years of experience running the Federal Employees Health Benefits (FEHB) Program. I do not see that the Multi State Programs have anything extra than the others. See also Minimum Essential Benefits and Medical Mandatory Loss Ratio’s
Consumer Resources & Links
- Here’s Provider Lists from ALL companies.
- Blue Cross SERVICE Phone # (800) 333-0912 or 310.519.1335
- Which Blue Cross Anthem Plans are Grandfathered?
- What are Multi State Plans?
- Blue Cross Wellness Programs
Anthem Blue Cross Grandfathered PLans being #discontinued!
- grandfathered clients enrolled on the Basic 2500 contract codes R418 & R419 that their plan was discontinued as of 6/1/24 and that they needed to choose an ACA medical plan.
- Anthem Blue Cross will be discontinuing the grandfathered plans below, the rest of their plans are good. The last day of coverage for these plans is December 31, 2022.
- Contract Code Plan description
- 1518 Basic 1000
- 7900 Basic 1000
PE25 Basic 1000
PE26 Basic 1000
- 7900 Basic 1000
- Z165 SmartSense 2500 Full RX
- Z166 SmartSense 2500 Full RX email dated 6.23.2022 *
- Anthem Blue Cross will let you know your options sample letter for selecting a new plan during
- 1518 Basic 1000
Blue Cross doesn't have any downgrade options - that is, the ability to just select a different grandfathered plan. You'll have to
Affected members will still receive rate action notifications through the end of the year.
- Old Brochures
- Our main webpage for Blue Cross Individual
Anthem Blue Cross
COVID Resource Center
Coverage of COVID 19
Rev 8.2020
10% premium discount for August 2020
More COVID FAQ's
Email us, if any links require a password











Can IBM retirees stay on the same Anthem Blue Cross Plan F insurance instead of having to get United Healthcare Advantage Plan? Thank you.
Please send me the URL Internet address and/or all the materials that HR gave you on your plan choices.
Am I financially better if I want to change to Anthem blue cross PPO at the same level of coverage I currently have. [Gold]
Watch this video we just made to help answer the question.
https://youtu.be/aZQzZuGi9VM
Steve,
Thanks for taking such good care of us.
You are really a great person in a sea of confusion .
Your loyal client,
Mike
1 I was interested in an anthem blue cross d [direct – not through Covered CA] platinum plan….
2 I have a cancer and
3 I did not have insurance previous. ….
4 is there a waiting period for my treatments
1. Great. See above links to get quotes.
2. I’m sorry to hear that. Hope you recover soon. Under Health Care Reform, there are no medical history questions. Section 2701.
3. That doesn’t matter either.
4. No. If you enroll by the 29th at 4 PM you can have coverage starting March 1, 2016. – While the official deadline is the 31st, we are not planning to work the weekend. Mental Health is also an essential benefit.